The (nearly) bionic woman
Posted: November 4, 2015 Filed under: Surgery | Tags: bionic knee, carpal tunnel, cubital tunnel, gen pop, post-mastectomy infection, PRP, Synthetic synovial fluid, Synvisc, Tommy John, total knee replacement, ulnar nerve transposition, Wonder Twins 8 CommentsI haven’t written much about surgeries lately. Well, truth be told, I haven’t written much about anything lately. But certainly not about surgeries. Despite the double-digit number of surgeries I have had in the last five years, I don’t like being cut upon or tweaked or refined. I’m good with my rough edges. My body has other ideas, however.
At the beginning of this year I had reached my limit of tolerance for the carpal tunnel pain & suffering so I consulted a well-respected hand specialist and got a nasty surprise. In addition to carpal tunnel, I also had cubital tunnel syndrome (I’m an overachiever that way), so the no-big-deal surgery to correct the issues in my right wrist morped into a full-blown ulnar nerve anterior transposition. It looked like this:
Yuk.
Long story short, the ulnar nerve (which runs from one’s neck to fingertip) becomes dislodged and gets caught on the bony ridge of one’s elbow when one stretches or bends at the elbow. Once dislodged, the nerve needs help getting back in the right place. So, my surgeon had to dig a new channel for my ulnar nerve to lie in, then stitch the nerve into the muscle to ensure that it didn’t go rogue again. It was as pleasant as it sounds (not really pleasant at all). And the scar is about as pretty as you might expect (not really pretty at all). It’s a good conversation piece, though; I’ve been asked more than once if I had Tommy John surgery (do I look like a baseball pitcher?) or whether I won the knife fight. 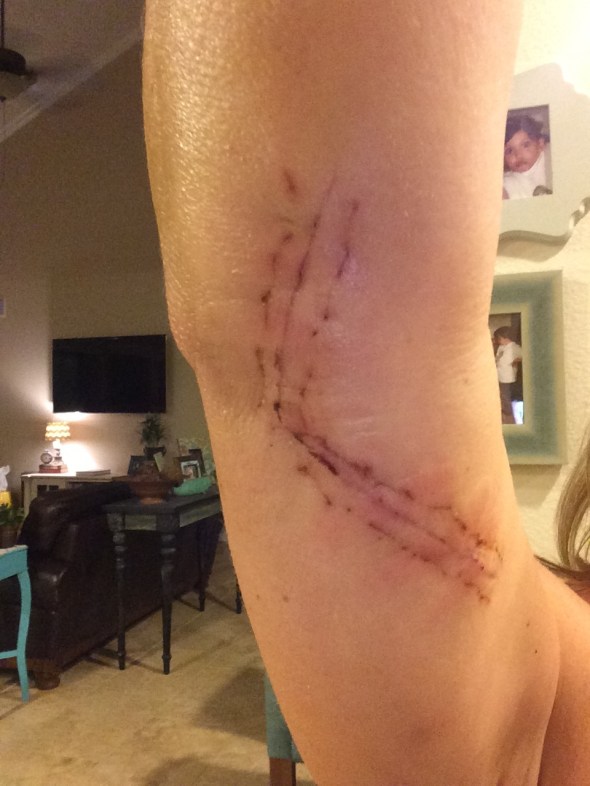
Now that I am recovered from the fun & games of my arm surgery, it’s time to get back on that OR table and get myself a new knee. Yes, a total knee replacement at the ripe old age of 46.
Don’t be jealous.
I’ve been dancing around the knee issue for years. After two arthroscopies, a lateral release and minor ACL repair, a PRP infusion, and 11 injections of synthetic synovial fluid in the last 10 years, it’s time. The x-rays that show zero cartilage say it’s time. The grinding of bone on bone say it’s time. The uncertainty of being able to get up from a crouched position say it’s time. The increased pain, decreased mobility, and off-the-charts frustration say it’s time.
Sigh.
Big sigh.
I’m not looking forward to this.
That said, I am intrigued by the particulars of an artificial knee; the one I’m getting is cutting-edge. It uses a proprietary Oxinium (oxidized zirconium) on the femoral part of the joint, a PMMA plastic on the tibial side, and a stainless steel piece to add a little sparkle. That oxinium is pretty cool; it’s a metal alloy that once heated transforms into a smooth surface that is super resistant to wear & tear and is much lighter than the metal used in older versions of knee replacement devices. It is free from nickel but will likely still set off the metal detectors at the airport. Fingers crossed that the TSA person who gives me a pat-down is gentle (and cute).
The combo of Oxinium and PMMA plastic are the Wonder Twins of knee replacement devices. Rumor has it this combo can last 30 years. That’s important when one is on the flat end of the bell curve that represents the average age of a knee-replacement recipient. As is my custom, I’m way ahead of my peers in my medical needs. Like 20 years ahead.
Being the weirdo that I am when it comes to surgeries, I like to gather all the gory details about the procedure. I usually watch a youtube video of an actual procedure, too, but usually after I’ve endured the horror of the real thing. Here’s how it will go down: Amy doc will make a vertical incision, probably between 6 and 10 inches, on my bum leg. Once in, he will move my kneecap so he can get to the leg bones. He’s going to cut my femur and tibia (if you’re strangely curious as I am, may I suggest that you don’t google “orthopedic bone saw?” That’s just creepy. The fact that such tools are available for purchase on eBay is even more creepy). He promised to measure twice and cut once. (Because the pieces that comprise an artificial knee come in some 90 sizes, I hope he measures more than twice!) Once the bones are cut, he will shape them to accommodate the new pieces that will make up my bionic knee and will attach the pieces to the bones. Then he will attach the parts to the kneecap, using bone cement. My doc told me that waiting for the cement to dry takes nearly as long as the rest of the procedure. Then he will sew me back up and once I’m awake and somewhat coherent, I’ll be off to my hospital room.
Most patients stay three nights in the hospital, but I’m already hoping to ditch out early. I’ve spent enough nights in the joint. I’m fortunate that my doc has a swanky surgery center not far from my home. There are only 5 rooms, which is good because I have no business mixing and mingling with the gen pop in a regular hospital. I hear a lot of people get really sick in hospitals.
World Cancer Day & Stuart Scott
Posted: February 4, 2015 Filed under: Uncategorized | Tags: Every Day I Fight by Stuart Scott, Jimmy V, Jimmy V Award for Perseverance, mycobacterium fortuitum, nosocomial infection, post-mastectomy infection, Stuart Scott, World Cancer Day 2 CommentsToday is World Cancer Day, and rather than rehashing my own cancer “journey” I’m thinking about Stuart Scott.
A longtime ESPN anchor, Scott was a familiar presence in my house. His wordsmithing appealed to me, as did his irreverancy. In a world populated by former jocks and professional windbags, Scott contributed a cool combination of intellectual breadth and liveliness. Scott’s colleague Dan Patrick once said about Scott that “he didn’t just push the envelope, he bulldozed the envelope.” I’m a fan of bulldozers.
Scott was diagnosed with appendix cancer in 2007. Yes, you read that right: appendix cancer. Weird and rare, there are an estimated 1,000 cases of appendix cancer in the United States annually, compared to nearly 300,000 cases of breast cancer every year in this country. Perhaps this is another reason I relate to Stuart Scott: between his appendix cancer and my post-mastectomy mycobacterium infection, we both faced the question of “who in the world contracts that??”
Stuart Scott wrote a book about his cancer “journey,” which explains his gladiator approach to confronting his disease. The cancer community is divided on the “battle” aspect of the cancer fight — some people love the idea of a cancer warrior while others are uncomfortable with the war metaphors — but one thing I know for sure: the cancer experience is a fiercely personal one, and no one has the right to tell another how to do it or which analogies to use.
I read an excerpt of Scott’s book and am hungry for more. He was a gym rat, like me, and he leaned heavily upon his workouts during treatment, both for physical strength and for mental health:
“I can’t tell you how important it felt to go from the chemo infusion center to the gym. There were patients at the infusion center who were gaunt and too weak to walk. I wanted to hug them. I wanted to work out for them. It took about fifteen minutes to get to the gym from the infusion center, but I felt like I was traveling a great distance: from the land of the sick to the land of the recovering. I’d work out three or four times a week, but the most important workout was the one right after chemo. It was like I was proving a point: While you kick my butt, cancer, I’m gonna kick yours.”
In thinking about the name of one of the drugs in his chemo cocktail, Scott realized “The medical name of the medicine is fluorouracil, but they call it 5-FU. That’s what it said, right there: 5-FU. All right, I thought. A sign. FU, cancer.”
FU cancer. Indeed.
Scott continues: “My return to the gym felt kind of spiritual. I wasn’t really supposed to run since I was still connected to the port that was giving me my medicine. I looked down, and my eye caught the logo of the manufacturer of the machine I was on: LifeStyle. That word jumped out at me: Life. I thought back to the first thought I had when [diagnosed]: I’m going to die. But I was still here. And here I was, not forty-five minutes out of chemo, and I was in the gym, doing what I do. I started to run. What could be the harm? The disease wasn’t in control. I was.”
That sense of control is of epic importance in the cancer “journey.”
Scott explains it like this: “Mentally, I needed to be in that gym. I’d talk smack to cancer like Ali talked to his opponents. A third set of push-ups? Take that, cancer. Twenty full-out sprint pass patterns? Cancer, you ever run up against this? Some kicks and punches into the middle of the heavy bag after the elliptical? I got yer cancer right here! I needed to do that, not just to show my girls I was fighting for them, but also to show myself I had some control over the situation. ‘Cause cancer wants to take control from you. You’ve got to very purposefully stand your ground. That’s what going to the gym is to me. I decide, cancer.”
A few weeks ago I came across the late ESPN sportscaster’s speech about his cancer “journey” at the ESPY awards last summer. That speech is powerful. Here’s the link so you can check it out.
Scott was awarded the Jimmy V Award at last year’s ESPYs and joins an acclaimed list of courageous and inspirational people from various corners of the sports world. Perhaps his career as an on-camera personality gave him the extra flair that made him such an engaging speaker. Maybe that was just his personality. Either way, his speech is compelling.
The take-away message, for me, lie in these words from that speech:
“When you die, that does not mean that you lost to cancer. You beat cancer by how you live, why you live and in the manner in which you live.”
Stuart Scott taught me a huge and valuable lesson. He did die, but he did not lose. How he lived proves that. Today, on World Cancer Day, I honor Stuart Scott. While at the gym, I will think of his no-mercy approach. I will remember all the days in which I was that patient too weak to walk, and I will silently thank him for all the times he worked out in my stead. For all the times he went straight from chemo to the gym and said FU, cancer.
#nofilter
Posted: November 6, 2014 Filed under: Uncategorized | Tags: carpal tunnel syndrome, Dog from Up, funny bone, micobacterium fortuitum, nerve conduction velocity test, neurological testing for ADD, post-mastectomy infection, PTSD, PTSD from cancer, Squirrel! 10 CommentsWhat kind of moron schedules an appointment with a new specialist while recovering from yet another revision to breast reconstruction? Probably the same moron who thinks yet another revision is no big whoop and expects recovery to be swift. Will I never learn??? And the post-surgery antibiotics are wreaking their usual havoc and using black magic to cause me — a non-meat-eater and pet-pig owner — to crave ham. Ham. Of all things.
Dr E, the neurologist I saw yesterday for the mystery neuropathy I’ve been having in my hands, offices in the medical plaza adjoining the hospital to which I was admitted in early June 2010 for the nefarious post-mastectomy infection. A small PTSD episode may or may not have occurred inside that plaza at 8:30 a.m. yesterday, in which I stepped on to the wrong elevator en route to Dr E’s office and found myself not in the plaza but on the 9th floor of the hospital. I was transfixed and rooted in place, knowing I was not in the right spot but temporarily unable to grind the right gears and get out of there. I stood there, sweating profusely and shivering alarmingly near a giant window overlooking the freeway that leads from the hospital back to my home, in the Land of Sugar. The dregs of a rainy-day morning rush hour in Houston creeped along that freeway as I watched it, momentarily paralyzed with the searing memory of looking out that window on day 6 or 7 of that hellish hospitalization. My kids had just finished their second- and fifth-grade years of school; I had turned 41 just a week before that hellish hospitalization. Summer glistened ahead of us as I began a protracted and ugly battle against a rare and nasty infection following a cruel and unexpected cancer diagnosis. If someone had predicted that nearly 5 years later I would be paralyzed simply by being in that same hospital, I would have rolled my eyes and scoffed at that lame-0 idea. Suffice to say, no eye-rolling or scoffing occurred.
 I sweated and cursed the small, airless room. I wondered how much time had elapsed. I wondered if clicking that button was contributing to the neuropathy in my hands. I rebelled against the test directions to avoid looking for a pattern and guessing when to click the button. I composed a grocery list. I fashioned a crude fan from a piece of paper to stir the hot, stale air, not once taking my eyes off that blasted screen. I thought about what to serve my kids for dinner that constituted a nutritious meal yet required little or no work from me. I vowed to ace that test, but grew bored of and distracted from it post haste. Hence the no filter.
I sweated and cursed the small, airless room. I wondered how much time had elapsed. I wondered if clicking that button was contributing to the neuropathy in my hands. I rebelled against the test directions to avoid looking for a pattern and guessing when to click the button. I composed a grocery list. I fashioned a crude fan from a piece of paper to stir the hot, stale air, not once taking my eyes off that blasted screen. I thought about what to serve my kids for dinner that constituted a nutritious meal yet required little or no work from me. I vowed to ace that test, but grew bored of and distracted from it post haste. Hence the no filter.But instead, I was like this (pardon the profanity; it’s fitting and again, another example of me having no filter):
The wrong approach?
Posted: August 17, 2014 Filed under: breast cancer, Surgery | Tags: breast cancer in young women, cancer of the nipple, CPM, gut instinct, infectious disease, JP drains, micobacterium fortuitum, Paget Disease, post-mastectomy infection, prophylactic mastectomy 7 CommentsIn this article for The New York Times, Peggy Orenstein addresses one of the many tricky topics surrounding breast cancer: to remove or not remove the “unaffected” breast?
It’s a tricky topic because the research and prevailing medical consensus are in direct opposition to gut instinct. Research says a bilateral mastectomy in patients with cancer in just one breast has little impact on survivability. Doctors say the odds of surviving low-grade noninvasive breast cancer is the same whether we undergo a lumpectomy or a mastectomy. But our guts often say “lop em both off.”
That’s what my gut told me to do, even after extensive research and number-crunching. My gut instinct leaped immediately to a slash-and-burn tactic. My darling breast surgeon required me to wait at least 3 days before making my decision on the lumpectomy vs mastectomy debate; I complied but my decision was made in the first 10 minutes of grasping my diagnosis. My gut told me to opt for the bilateral mastectomy.
I suppose this puts me in the category of women opting for a CPM, or contralateral prophylactic mastectomy. The experts whom Orenstein spoke to about the CPM debate refer to the increase in women undergoing CPM as “epidemic” and “alarming” and believe it is driven by women not fully understanding the math. Girls have always been bad at math, right? That’s the message I got, growing up in the 1970s in suburban America.
A 2013 study done by Boston’s famed Dana-Farber clinic revealed that women younger than 40 with no increased genetic risk who had cancer in one breast believed that “within five years, 10 out of 100 of them would develop it in the other; the actual risk is about 2 to 4 percent.”
Upon my diagnosis, I understood the math. It wasn’t easy and it was confusing. It took time and effort, but it was not beyond me (having a math guru in the house helped tremendously, but the point still stands). I understood that my chances of successfully removing the cancer in my “affected” breast was the same whether it was done via lumpectomy or mastectomy. I understood that my chances of developing the same cancer in the other breast were slim to none, because, as Orenstein says,”cancer doesn’t just leap from breast to breast.” I understood that low-grade noninvasive lazy cancers don’t typically become deadly; it takes a cancer that metastasizes to do that.
I also understood that a bilateral mastectomy is not an easy surgery. Not by a long shot. As Orenstein so colorfully describes it, “breasts don’t just screw off, like jar lids.” Undergoing a mastectomy involves not only losing the breast itself but also (typically) the nipple and areola, as well as the lining of the chest muscles. Factor in the JP drains that are snaked into the traumatized chest, just to add insult to injury. I couldn’t lift my arms for days after my mastectomy and needed help with the simplest things, such as brushing my teeth and applying chapstick. I needed a new, temporary wardrobe of tops that buttoned or zipped up, because lifting my arms over my head to put on or take off a shirt was a no-go for my battered upper body. I needed help — lots of help — which doesn’t jive with my stubborn and independent countenance.
I knew that choosing the harder road of a bilateral mastectomy over the easier, less-invasive lumpectomy did not increase my odds of surviving breast cancer. At least according to the studies. I knew that a mastectomy is much riskier than a lumpectomy. I knew that recovery would be much harder and more time-consuming. Nonetheless, my gut told me to take that more difficult road. My gut was right.
Orenstein spoke to Steven J. Katz, a University of Michigan professor of medicine and health management. He studies medical decision-making, and has found that people tend to react from the gut when confronted with a diagnosis because we are wired to make “fast-flow decisions” that make us want to flee. Understandable to anyone who has been on the other side of the doctor delivering bad news. Upon diagnosis, Orenstein recalls feeling “as if a humongous cockroach had been dropped onto my chest. I could barely contain the urge to bat frantically at my breast screaming, ‘Get it off! Get it off!'” Her version involved a giant cockroach; my version involved a scorched earth.
Dr. Katz says that doctors need to understand how our gut reaction affects our post-diagnosis decision. He speaks of “the power of anticipated regret: how people imagine they’d feel if their illness returned and they had not done ‘everything’ to fight it when they’d had the chance. Patients will go to extremes to restore peace of mind, even undergoing surgery that, paradoxically, won’t change the medical basis for their fear.”
It is a paradox: our intellectual self versus our gut.
Orenstein points out that “it seems almost primal to offer up a healthy breast to fate, as a symbol of our willingness to give all we have to and for our families. It’s hard to imagine, by contrast, that someone with a basal cell carcinoma on one ear would needlessly remove the other one ‘just in case’ or for the sake of symmetry.”
While it may be hard to imagine, there’s no way to predict how one will react to a cancer diagnosis. All the studies and statistics are worthless in the face of the worst-possible scenario, which is facing cancer. I was 40 years old, with 2 kids under the age of 10, when I faced that scenario. Of course I thought of them and the possibility of leaving them motherless and rudderless. Having lost my own sweet mama brought that into even clearer focus. Perhaps my decision to undergo a CPM was based more on emotion than on rational thought. No doubt my gut was driving that bus.
But guess what? My gut is a careful and prescient driver. In steering me toward the more-radical surgery option, my gut saved me. Maybe saved my life, but definitely saved me from undergoing a second mastectomy, one that would most definitely not have been of the CPM variety.
My “unaffected” breast had cancer, too. And Paget disease to boot. Nothing had showed up on any of the myriad tests or scans I’d had before my mastectomy. It was the surgical pathology on the “unaffected” breast that finally revealed those cancers. How long would those cancers have grown, unannounced and unaccounted for, had I not followed my instinct and listened to my gut? I don’t like to think about that.
I’ve learned — the hard way, of course — that I’m one of those medical weirdos whose body does not conform to standard protocols. I’m the kook who gets the weird stuff; to wit, Paget disease accounts for a mere 1 to 4 percent all breast cancers, according to the National Cancer Institute. Ditto the post-mastectomy infection I contracted. Who gets a microbacterium fortitum?? So few people that my infectious disease team — yes, I had a team of ID docs — still wonders where the hell that originated.
We medical weirdos don’t fit into studies or facts or figures. We are the ones who keep their doctors up at night, scratching their heads and wondering what?? what?? what is going on here?? We are the ones for whom the “if it can go wrong, it will” axiom applies. We are the ones who make other people reassess the shittyness of their situation (you’re welcome, by the way).
We are the ones who follow our gut and don’t look back. Is that the wrong approach? Not for me. 
World Cancer Day
Posted: February 4, 2014 Filed under: Uncategorized | Tags: cardio intervals on the VersaClimber, motivational posters, mycobacterium, mycobacterium fortuitum, nosocomial infection, post-mastectomy infection, Sir Edmund Hillary, VersaClimber, World Cancer Day 1 CommentToday is World Cancer Day. This year’s theme is debunking myths and erasing stigmas attached to cancer. While I’m all for the debunking and erasing, I’m not at all sure how to feel about cancer having its own day. At first blush, I thought: Woohoo! A day to celebrate! I’m always up for that. But then I thought, Wait: what exactly am I celebrating? The fact that I survived? No; too much emphasis on survival makes me uncomfortable, as if I’m tempting fate. The fact that there’s so much awareness and dialogue about cancer nowadays? No; I’m sick of talking about it and even more sick of thinking about it. The fact that I persevered despite a devastating illness and an even more dangerous nosocomial infection? No; I would have rather skipped the whole experience. Especially the infection part.
Not knowing exactly what to make of this day, I’ll focus on this:
There’s a poster at my gym with this quote from Sir Edmund Hillary. I’m assuming it’s in reference to Mt Everest. I look at the poster when I’m on the VersaClimber — a cardio machine that at first seemed like an instrument of torture but now is part of my routine. Most times I have to close my eyes to get through my VersaClimber intervals (it’s pretty bad!). But when I’m not closing my eyes, I look at the poster and read Hillary’s words, and realize that indeed, we do conquer ourselves. Including the cancer.
PSA, from me to you. You’re welcome.
Posted: November 30, 2012 Filed under: breast cancer | Tags: breast cancer in young women, breast reconstruction, DIEP reconstruction, Hibiclens, micro-mini pigs, mini pigs as pets, miniature potbellied pigs, Oncotype, post-mastectomy infection, the Big Dig 14 CommentsFrom time to time, I like to provide a public service announcement for the greater good. In other words, I learn the hard way — the expensive way — and share my lesson in hopes that some diligent reader out there in the blog-o-sphere heeds my words and avoids the painful/stressful/costly conundrums in which I tend to find myself.
Today’s PSA does not concern courteous driving (although perhaps it should, based on the overwhelming number of idiot drivers I’m surrounded by every time I venture out of my house). Today’s PSA will not address healthy living or how to fortify your liver for maximum alcohol consumption. Today’s PSA won’t even mention Pinktober, pinkwashing, or how misguided The Susan G Komen for the Cure organization has become. Today’s PSA doesn’t have anything to do with our little piggie (pity that, as she is infinitely entertaining).
Today’s PSA is all about how your health insurance company can — and likely will — try to screw you with the whole in-network/out-of-network debacle. 
I recently had a surgery that, lo and behold, had absolutely nothing to do with breast cancer or breast reconstruction or breast reconstruction revision. How refreshing! I did my due diligence in researching a specialist who was the right guy for the job. I asked before I even made the appointment if he accepted my insurance. I provided all the nitty-gritty details insurance details before I saw the doc (ID number, group number, 800 number for claims). The benefits coordinator at the surgeon’s office reviewed everything on her checklist and assured me that we were good to go.
I saw the doc, he confirmed that the surgery was medically necessary and with just cause, and we scheduled a date. I paid my co-pay for the office visit and filled out all the paperwork, including multiple recitations of the insurance company details. I paid for my portion of the surgery well in advance. I followed all the rules (so I thought), and like a veteran soldier readying for battle, I eschewed any aspirin or blood-thinning products that can promote bleeding during surgery; I drank plenty of water the day before surgery to aid the anesthesiologist in finding a good, plump vein; I ate a healthy meal that would hopefully see me through being NPO the night before surgery; I washed the area to be sliced & diced with Hibiclens in my paranoid ritual of warding away any bacteria that might host a party in my surgerized body; I procured prescriptions in advance for the 2 antibiotics that are forever a part of my arsenal since that pesky post-mastectomy infection; I showed up before the crack of dawn on surgery day with an empty stomach and a powerful ache for my usual cup of coffee. I know the drill; been there, done that, multiple times. I got this.
Surgery was uneventful, recovery was long for my impatient self, but there were no complications.
Until I got a bill from the surgery center for more than $20,000.
20,000 clams for a surgery that was on the up-and-up and had been cleared for take-off well in advance.
Say what?
After suffering a minor heart attack, I called the surgery center and was told to take it up with my insurance company. I called my insurance company and was told to talk to the doctor’s office. I called the doctor’s office and was told to retrace my steps and start over with the surgery center. Egads.
After spinning my wheels and listening to untold atrocious Muzak songs while on hold for what seemed like forever, I remembered that my insurance company provides a patient advocate service. I’d used this service with my previous insurance company and was forever grateful for my advocate, a former RN, who checked in on me post-mastectomy and throughout the course of the year-long infection battle. She intervened when the insurance company said it didn’t want to pay for the $5,000 Oncotype test, which dissects my particular cancer to determine the best way to treat it and determine how likely it is to recur. She helped me navigate the pages upon pages of medical bills that weighed down my mailbox in the early stage of my cancer “journey.” She was very helpful.
The new insurance company could take a lesson from her. Their patient “advocate” department sucks. I can barely stand to use the word advocate in relation to them (hence the quotation marks).
The first “advocate” I dealt with on this issue did some research and determined that the surgery center my in-network doctor used is out-of-network. So my surgeon is in-network but the surgery center is not.
Huh??
Oh, and by the way, it’s my responsibility to check to be sure the surgery center is in-network.
Again I say Huh??
After all the checking and double-checking and verifying and pre-qualifying and certifying, I’m supposed to ask about the surgery center? How in the world would I even know to ask about this? What fresh hell is this?
Oh, yes indeedy, the “advocate” told me, I should have checked on that. And I should have known to check on that by reading the Standard Plan Description, a bazillion-page online document that details the ins and outs of my coverage.
While I’m grateful for the coverage I do have, I’m pretty sure my insurance company hates people like me who ring up millions of dollars in expenses for a disease they did nothing to cause and for which they actively tried to prevent. I imagine my file has a big red X on it to denote all the trouble I’ve caused and money the company has had to spend on my behalf. I’m guessing that when I call the insurance company with a question, the phone has a special ring, sorta like the Bat-phone, to alert the poor sap who answers it that I’m a raucous troublemaker who is bleeding their employer dry.
I get it. I’m not the ideal customer. But expecting me to verify that the surgery center is in-network is absurd. I don’t care what the bazillion-page online document says. If the doc is in-network and no one raises a red flag about the surgery center, then I assume I’m all clear.
A $20K bill and an instant heart attack are rather the antithesis of all clear.
And that, dear readers, is why I’m here today — to lead by example, to inform by the hard lessons learned. The word to the wise, learned expo-facto, is this: even if your doc is in-network, the surgery center may not be. Even if the doctor’s office staff have dotted every i and crossed every t, it may not be enough. Your insurance company my turn on you like a hungry dog on an alley chicken-bone and try to chew you up and spit you out. Consider yourself forewarned.
Odd girl out at the oncology office
Posted: July 11, 2012 Filed under: breast cancer | Tags: cancer battle, getting back to normal after cancer, life after cancer, post-mastectomy infection, psychological effects of cancer, PTSD, survivor's guilt 31 CommentsI’ve been on hiatus from blogging but rest assured, all is well. No real reason for the hiatus other than the fullness of life. Although I’ve not been wrapped up in the hurried pace of the school year, so far summertime finds me still going & blowing as usual. Less than three weeks until our annual vacation to Salisbury Beach, though, and I will slow down then. As the sage Zac Brown says, I’ll have my toes in the water, ass in the sand, not a worry in the world, a cold beer in my hand. Can’t wait.
Yesterday was my quarterly check-up with my cutie pie oncologist. My intrepid appointment companion Amy is currently living the good life seaside on the East Coast, so I had to go it alone. She strongly suggested I reschedule, lest she miss a visit with Dr Cutie, but alas, I carried on without her. She’ll have to wait until November to lay eyes on him, as I’ve graduated to three visits a year with him. That’s my reward for being two years out from the dreaded disease: fewer oncology appointments.
Despite one fewer chance a year to gaze upon Dr Cutie as he imparts his wisdom, this is a good thing because I found myself feeling guilty sitting in the waiting room. Of the four other patients waiting for the good doctor, I was the only one with hair. The others were not only bald but quite sickly looking (and a good 20 years older than me, as well). As I perched on a chair in my workout clothes, planning to hit it hard at the gym as soon as I got the requisite visit out of the way, I was filled with a sense of guilt over my good health.
I could feel the eyes of the other patients on me, and I imagined them wondering, as I would in their shoes, what a strapping gal with a full head of hair, color in her cheeks, and a spring in her step was doing at an oncologist’s office. Had the shoe been on the other foot, I would have assumed this picture of health was meeting someone there, or perhaps had found herself in the wrong office and had not yet realized the mistake.
My guilt was somewhat assuaged by the stark recollection that there was a time, not so long ago, when I was the sickly looking one, dragging myself from one appointment to the next, consumed with healing after a double mastectomy and overwhelmed by a post-surgical infection. I remember well the days of envying the “normal” people who walked with ease and were unburdened by the pressing concerns of cancer, treatment, and their ugly fallouts. Ditto for all the days (close to 30 days all told that one summer) I spent in the hospital. Pushing my IV pole on endless loops around the hospital halls, I would gaze longingly at the healthy people out and about and wish I were among them.
Although I’m two years out from the dreaded disease (or, two years and 2 months, as Dr Cutie so astutely recited from memory), the recovery process from the infection was quite lengthy, and it’s really not been all that long since I was freed from the clutches of that wretched bug. Many times as I moved from the infectious disease team’s office in the Texas Medical Center to Dr Cutie’s office around the corner from home and to the plastic surgeon’s office halfway in between the two, I stared hard at the healthier specimens I saw along the way. I remember feelings that ranged from outright envy to smoldering anger at these people who went about their daily business the way I used to. I envisioned these people getting their kids off to school, hitting the gym, running errands, lunching with friends, and doing household chores with ease, the way I used to. I imagined the fabric of their lives being uninterrupted by cancer, the rudest of guests, and assumed that they sailed through their days focused on minor inconveniences rather than big-time medical crises. First-world problems like a cancelled hair appointment or a rained-out tennis match were screechingly replaced by real-world problems like a hole in one’s chest wall that just won’t heal and an insidious bacteria that evades treatment quite stealthily.
Was it survivor’s guilt that hit me yesterday in the doctor’s office? Perhaps. I’ve never been one to wonder “why me?” — neither in terms of the roulette wheel of whose genes will come up hinky and necessitate a diagnosis, nor in terms of why am I now healthy while so many others are sick. Seems like a colossal waste of time and energy to me. I don’t spend much time thinking back about the sheer hell I endured with that nasty infection; partly because I don’t want to go there, and partly because my brain works hard to protect me from going there. There are plenty of gory details I have to work hard to conjure up, and while my intellectual brain knows that of course I did go through all that, my sympathetic brain says let’s not rehash that ugly past and prevents me from really remembering how awful it was. Better to smile encouragingly at the other patients in the waiting room and spend a few minutes of quiet reflection on the road I’ve traveled and how far I’ve come.
These baseball years
Posted: July 3, 2012 Filed under: baseball | Tags: baseball memories, baseball-themed bedroom, First Colony Little League, Little League baseball, post-mastectomy infection, Southern Living magazine, Texas baseball, youth sports 19 CommentsOn my bulletin board I have a faded article from Southern Living magazine titled These Baseball Years. It’s from the June 2003 issue, when my son was four years old and just dipping his toe in the water of what would become a full-fledged baseball obsession. Now, 9 years later and in his last hurrah of Little League, I re-read the article and nodded my head in agreement.
Baseball has been a constant in our house, and it’s provided me a way to connect with my kid, who tends to be rather quiet and lives in his own head. He’s never been one to come home from school with news of the day’s events, nor does he disclose much under direct questioning. If there were a hall of fame for one-word answers, he’d be in it.
All of that changed, however, when I realized that if I knew something about baseball, especially about his beloved Red Sox, I’d have a direct line into him. Any parenting expert will tell you that if you want to connect with your kids, you have to do it at their level and with their interests in mind.
In the article, author Joe Rada says that “baseball is a grand metaphor for the game of life. Through baseball we explore the weighty issues of winning and losing gracefully; getting along with others; setting goals; playing hard and by the rules; rolling with the punches; the value of physical health and the treacheries of drug abuse.”
He also describes how his son sleeps on baseball-themed sheets under a ceiling fan with baseball-bat blades. Sounds familiar. At the time when I ripped the article out of the magazine, my kid slept on sheets decorated with cars & trucks, but it wasn’t long before we re-did his room with a baseball theme. We chose the neutral brown paint color for his room based on which shade was closest to infield dirt, and the one accent wall we painted red was carefully matched to the Red Sox jerseys. His ceiling fan is regulation, but his lamp and his curtain tie-backs are baseball-themed. As he moved through Little League seasons, we added shelves to hold trophies, and now I’m worried those shelves will collapse under the weight. 
This last season of All Stars is the end of an era. We’ve spent as much time in the stands as we have around our dinner table, and we’ve bonded with the other players’ families in a friends-for-life kind of way. We’ve seen each other through job loss, injuries & illness, new babies, and high school graduations. We’ve supported each other through health crises, including my own. The summer I spent in the hospital instead of at the All Star games in 2010 was brutal, but it was made bearable by the love and support that came from the team. The Season of the Pink Sweatbands was the team’s best, and my framed photo of the entire team, including coaches, wearing pink sweatbands and saying “This one’s for you!” sat in each hospital room I occupied that summer. It remains one of my most treasured possessions.
 Like Joe Rada, we plan our family vacations around the baseball schedule, delaying as long as possible in hopes that we’ll be making a trip to the State Championship in late July before we take off for two weeks at the beach.
Like Joe Rada, we plan our family vacations around the baseball schedule, delaying as long as possible in hopes that we’ll be making a trip to the State Championship in late July before we take off for two weeks at the beach.
I don’t know why I kept that faded article all these years, but now that my kid is heading toward the end of his Little League career, I’m glad I did. As Rada writes, “Long after my son settles into being whatever kind of man he’ll be, I’ll still see his upturned chin and hear his sweet voice shouting across the backyard, ‘I got it!'” I will, too. 
Elizabeth Lloyd: you’re an idiot
Posted: June 27, 2012 Filed under: baseball | Tags: Elizabeth Lloyd, Little League baseball, micobacterium fortuitum, nosocomial infection, People I Want to Punch in the Throat, post-mastectomy infection, ridiculous lawsuits, the Big Dig 9 CommentsI’d use a more colorful name but she’d probably sue me. Like she’s suing an 11-year-old boy for throwing a baseball. In a dugout. At a Little League ball field, where presumably baseballs are thrown and sometimes not caught. But wait, if Elizabeth Lloyd has chosen to insert herself into the media, in her money-grubbing way, she’s a public figure, right? So I can call her whatever name I like and she has to take it. Perhaps I need to brush up on my libel knowledge, but in the meantime, I’m going to call her Asshat.
Here’s the story, in case you were paying attention to real news that actually matters and missed it: Asshat was at a Little League game in New Jersey two years ago, watching her son play, and was hit in the face by a ball. She was sitting on top of a picnic table next to the fenced dugout where a catcher, Matthew Migliaccio, was warming up his teammate, the pitcher. Migliaccio overthrew the ball and it hit Asshat in the face. According to the local newspaper, He ran over to her to ask if she was ok, and she told him she was fine. Says Matthew: “I went over to see if she was okay, and she said that she was fine and not to worry about it. About like three weeks after, she came and gave me a hug and she told me that it wasn’t my fault.” Asshat said to Matthew, “I know you didn’t do anything wrong.”
However, two years later — just days before the statute of limitations would expire — Asshat decides that errant ball was thrown “intentionally and recklessly” and she needs half a million dollars for it. WTH??
Asshat claims that Matthew assaulted and battered her.
WTH??
This claim is insulting to anyone who has truly been assaulted and/or battered. I’m sick.
So is Matthew. Poor baby was minding his own business, probably playing MW3 on the Playstation like the 13-year-old boy who lives at my house, when the doorbell rings and he is served papers. A 13-year-old child was served papers. Matthew said, “I think it’s pretty mean to sue someone after you told them that you knew it wasn’t their fault.”
Pretty mean indeed.
Matthew’s attorney, Anthony Pagano, says the case is bogus and the family will not settle with Asshat. “What are we gonna do, take his bike? He’s 11,” Pagano said.
Fact: 11-year-old kids overthrow balls. Fact: 11-year-old kids do not always catch overthrown balls. Fact: Elizabeth Lloyd is an asshat.
The overthrown ball traveled more than 60 feet before it hit Asshat, who was sitting 5 feet from the fenced bullpen. Reports conclude that while Matthew is an avid gamer, playing on 3 different teams, he was 11 years old at the time of the “assault” and didn’t exactly have a cannon of an arm like one sees in the major league. Matthew’s father says ”It’s absurd to expect every 11-year-old to throw the ball on target. Everyone knows you’ve got to watch out. You assume some risk when you go out to a field. That’s just part of being at a game.”
Hear hear. Guess what, Asshat — life is risky; get a helmet.