8 weeks later
Posted: January 3, 2016 Filed under: Surgery | Tags: acupuncture, Cryo Cuff, Graston technique, ice cast, knee replacement surgery, Kneehab XP, myofascial massage, physical therapy, PT, PT after TKR, recovering from knee replacement, total knee replacement, Venapro 21 CommentsFive and a half weeks. 37 days. A milestone — finally. My first real milestone after my knee replacement came on day 37 post-op. On that day, I woke up on my own instead of from pain.
In my last post about my knee replacement surgery, it was easy to imagine constant pain for 6 weeks post-surgery. While I’m happy to have noticed relief a few days shy of that, 37 days is a loooooooooong time to be in pain. And the pain isn’t totally gone, either. As I begin my eighth week with my new knee, I still have pain–especially during and after physical therapy–but it’s no longer my constant companion. 
I no longer walk with a limp, thankfully. I can go up stairs with relative ease, but coming down stairs is a different story. My new knee still doesn’t want to bend the way it needs to. It still barks at me and my unrealistic expectations. Even though I had read extensively about recovery and thought I knew what to expect, I had no idea how hard this would be.
If you happen to have a story about a neighbor/parent/spouse/boss who had a knee replacement and “was up and about like normal within a few weeks,” do not tell me about it. Just don’t. I don’t want to know. Yeah, yeah: everyone heals differently, it’s major surgery, anytime they cut your bones it’s a hard recovery blah blah blah. I know that. In my intellectual brain I know that. But in my crazy brain, I have this stupid idea that eight weeks is more than enough time to heal. Crazy Brain and I would like to get back to normal, please.
These days, my life revolves around physical therapy, my ice cast, the Kneehab XP, and a compounded antiinflammatory cream. Three days a week I spend an hour and a half at PT; on the days that I don’t attend PT, I do a series of exercises at home twice a day. Pedaling a stationary bike and doing squats are the least heinous parts of my PT. The Graston treatment falls into the heinous category. Graston involves the therapist using one of these tools to press, scrape, and apply pressure to the injured area. While it can hurt enough to induce a cold sweat and a string of curse words, it breaks up scar tissue adhesions, softens the fascia, and promotes healing. 
After the Graston treatment comes acupuncture. Graston breaks up the bad stuff and then acupuncture helps escort that bad stuff away from my knee and out of my system. Here’s hoping that Graston and acupuncture continue to combine WonderTwin powers to heal this mess. 
Once I get home from PT, I strap on my ice cast and wait for the cold to overpower the pain. Sweet, sweet relief. This thing is pretty great: the cooler holds ice and water, which flow into the leg cuff, along with air for compression. It gets cold quick and stays cold long enough to wipe out the damage done progress made at PT. If only I could figure out how to store a glass of champagne in the cooler when it’s not strapped to me.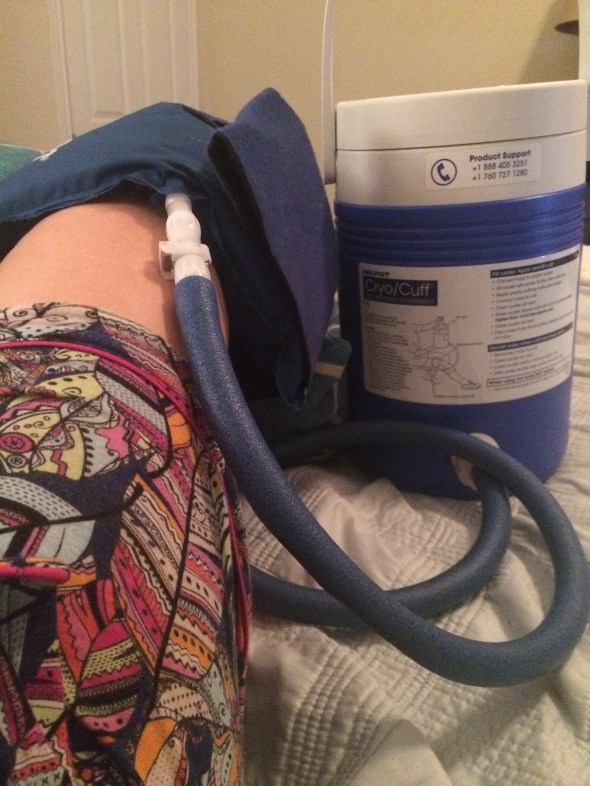
When I’m not icing, I’m firing up the Kneehab XP.  On the inside of this sleeve are electrodes that sit right on top of the affected area and deliver electrical stimulation to the quadriceps to force the muscles to contract. Those quad muscles have been underutilized because of the damage to my knee; by forcing them to engage, the Kneehab XP promotes strengthening and reminds those muscles to get back to work.
On the inside of this sleeve are electrodes that sit right on top of the affected area and deliver electrical stimulation to the quadriceps to force the muscles to contract. Those quad muscles have been underutilized because of the damage to my knee; by forcing them to engage, the Kneehab XP promotes strengthening and reminds those muscles to get back to work.
Here’s how the incision looks today. It too is healing, slowly slowly slowly. Much too slowly for me and Crazy Brain. 
The (nearly) bionic woman
Posted: November 4, 2015 Filed under: Surgery | Tags: bionic knee, carpal tunnel, cubital tunnel, gen pop, post-mastectomy infection, PRP, Synthetic synovial fluid, Synvisc, Tommy John, total knee replacement, ulnar nerve transposition, Wonder Twins 8 CommentsI haven’t written much about surgeries lately. Well, truth be told, I haven’t written much about anything lately. But certainly not about surgeries. Despite the double-digit number of surgeries I have had in the last five years, I don’t like being cut upon or tweaked or refined. I’m good with my rough edges. My body has other ideas, however.
At the beginning of this year I had reached my limit of tolerance for the carpal tunnel pain & suffering so I consulted a well-respected hand specialist and got a nasty surprise. In addition to carpal tunnel, I also had cubital tunnel syndrome (I’m an overachiever that way), so the no-big-deal surgery to correct the issues in my right wrist morped into a full-blown ulnar nerve anterior transposition. It looked like this:
Yuk.
Long story short, the ulnar nerve (which runs from one’s neck to fingertip) becomes dislodged and gets caught on the bony ridge of one’s elbow when one stretches or bends at the elbow. Once dislodged, the nerve needs help getting back in the right place. So, my surgeon had to dig a new channel for my ulnar nerve to lie in, then stitch the nerve into the muscle to ensure that it didn’t go rogue again. It was as pleasant as it sounds (not really pleasant at all). And the scar is about as pretty as you might expect (not really pretty at all). It’s a good conversation piece, though; I’ve been asked more than once if I had Tommy John surgery (do I look like a baseball pitcher?) or whether I won the knife fight. 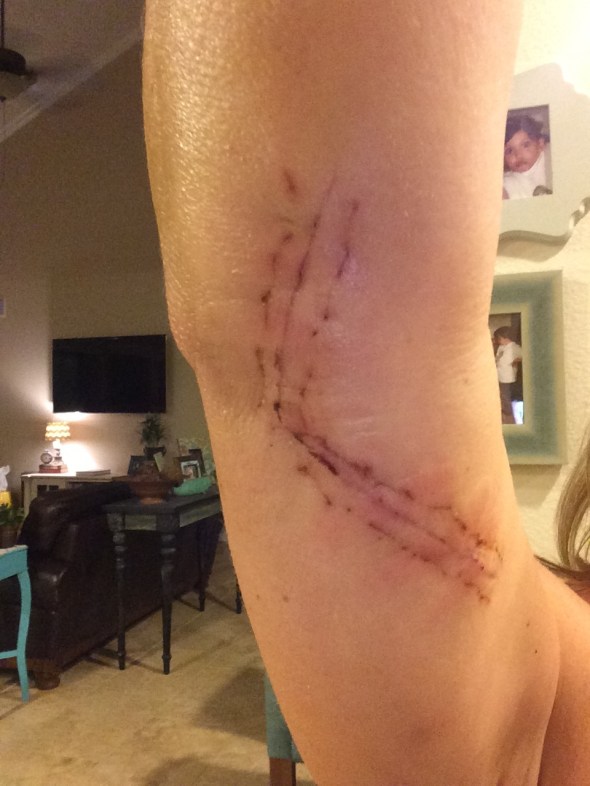
Now that I am recovered from the fun & games of my arm surgery, it’s time to get back on that OR table and get myself a new knee. Yes, a total knee replacement at the ripe old age of 46.
Don’t be jealous.
I’ve been dancing around the knee issue for years. After two arthroscopies, a lateral release and minor ACL repair, a PRP infusion, and 11 injections of synthetic synovial fluid in the last 10 years, it’s time. The x-rays that show zero cartilage say it’s time. The grinding of bone on bone say it’s time. The uncertainty of being able to get up from a crouched position say it’s time. The increased pain, decreased mobility, and off-the-charts frustration say it’s time.
Sigh.
Big sigh.
I’m not looking forward to this.
That said, I am intrigued by the particulars of an artificial knee; the one I’m getting is cutting-edge. It uses a proprietary Oxinium (oxidized zirconium) on the femoral part of the joint, a PMMA plastic on the tibial side, and a stainless steel piece to add a little sparkle. That oxinium is pretty cool; it’s a metal alloy that once heated transforms into a smooth surface that is super resistant to wear & tear and is much lighter than the metal used in older versions of knee replacement devices. It is free from nickel but will likely still set off the metal detectors at the airport. Fingers crossed that the TSA person who gives me a pat-down is gentle (and cute).
The combo of Oxinium and PMMA plastic are the Wonder Twins of knee replacement devices. Rumor has it this combo can last 30 years. That’s important when one is on the flat end of the bell curve that represents the average age of a knee-replacement recipient. As is my custom, I’m way ahead of my peers in my medical needs. Like 20 years ahead.
Being the weirdo that I am when it comes to surgeries, I like to gather all the gory details about the procedure. I usually watch a youtube video of an actual procedure, too, but usually after I’ve endured the horror of the real thing. Here’s how it will go down: Amy doc will make a vertical incision, probably between 6 and 10 inches, on my bum leg. Once in, he will move my kneecap so he can get to the leg bones. He’s going to cut my femur and tibia (if you’re strangely curious as I am, may I suggest that you don’t google “orthopedic bone saw?” That’s just creepy. The fact that such tools are available for purchase on eBay is even more creepy). He promised to measure twice and cut once. (Because the pieces that comprise an artificial knee come in some 90 sizes, I hope he measures more than twice!) Once the bones are cut, he will shape them to accommodate the new pieces that will make up my bionic knee and will attach the pieces to the bones. Then he will attach the parts to the kneecap, using bone cement. My doc told me that waiting for the cement to dry takes nearly as long as the rest of the procedure. Then he will sew me back up and once I’m awake and somewhat coherent, I’ll be off to my hospital room.
Most patients stay three nights in the hospital, but I’m already hoping to ditch out early. I’ve spent enough nights in the joint. I’m fortunate that my doc has a swanky surgery center not far from my home. There are only 5 rooms, which is good because I have no business mixing and mingling with the gen pop in a regular hospital. I hear a lot of people get really sick in hospitals.
New year, new game
Posted: January 19, 2015 Filed under: cancer fatigue, Surgery, Uncategorized | Tags: carpal tunnel syndrome, CTS and hypothyroid, hypothyroidism, lateral release for dislocated kneecap, Maque knee surgery, osteotomy, Supartz, Synthetic synovial fluid, thyroid biopsy, thyroid nodules 13 CommentsTwo weeks into this new year, I am wrapping my head around a whole ‘nother challenge. This new game has nothing to do with cancer (for the moment, anyway — knock wood) but concerns the myriad ways my body challenges me. I refrain from classifying those challenges as failures, i.e., the many ways in which my body is failing me, because that is the new game: the mental side of physical illness.
I’m a fierce player in all aspects of the game that is confronting health issues. All aspects except the mental game. I suck at that part. Give me the worst-case scenario (mycobacterium fortuitum, I’m talking to you) and I will slay it. Give me a long, difficult road on which to travel, and I will keep on truckin’. But tell me that the only weapon I have in which to fight is my mind, and I’m hosed. Tell me to stay positive and look on the bright side, and I struggle. Offer me platitudes and I will want to punch someone. Outlook: not great.
Some of the news ways in which my body challenges (fails) me are minor: graduating to the bifocal club, or needing to hit the hay well before midnight. To those challenges I say let’s call a truce. But the bigger challenges are well, bigger. And more challenging. There are three bad guys vying for attention these days: the bad knee, the wonky thyroid, and carpal tunnel syndrome. Awesome.
The bad knee is acting up and acting out. Again. Three surgeries and countless rehab exercises mean nothing to that old hag. The misaligned kneecap is screaming for attention, and the missing cartilage is hunkering for its piece of the pie. Two very squeaky wheels in an already crowded field. The second round of synthetic synovial fluid injections did little to appease the missing cartilage.  Despite the giant needle being jabbed straight into the innocent flesh adjacent to the bone-on-bone area, relief evaded me. Upon reviewing my day-after-Christmas x-ray, my orthopedist shifted gears from a previous recommendation of partial knee replacement to osteotomy, which requires cutting the bone at the top of the tibia and using plates and screws to relocate it in its proper place. The one word that comes up when researching the recovery for this surgery: brutal. Standard care is crutches for two weeks and a cane for a month alongside endless physical therapy. Thanks but no thanks.
Despite the giant needle being jabbed straight into the innocent flesh adjacent to the bone-on-bone area, relief evaded me. Upon reviewing my day-after-Christmas x-ray, my orthopedist shifted gears from a previous recommendation of partial knee replacement to osteotomy, which requires cutting the bone at the top of the tibia and using plates and screws to relocate it in its proper place. The one word that comes up when researching the recovery for this surgery: brutal. Standard care is crutches for two weeks and a cane for a month alongside endless physical therapy. Thanks but no thanks.
The thyroid is being an asshole, as well. Long story short: underactive thyroid, two daily meds, and two nodules that may or may not be problematic, and dissenting opinions by my crack medical team as to whether another thyroid biopsy is needed. Being the fierce player that I am, had my crack team concurred, I would have promptly had that biopsy. As much as I detest the idea of another needle being stuck IN MY NECK, I will do it if it’s necessary. But if there is dissent on the matter, I’ll defer. That said, that asshole thyroid has some wily ways of mucking up my life. Symptoms and side-effects of a wonky thyroid are far-reaching, and just when I think I have them under control (or am at least resigned to them), another one makes its grand entrance.
Which brings us to the third challenge: carpal tunnel syndrome. For a couple of years I’ve had what I thought was neuropathy: tingling, numbness, swelling, and radiating pain in both hands especially first thing in the morning. It came to a head shortly after we moved into our new house last year, and my GP chalked it up to overuse of my hands and forearms from packing and unpacking endless boxes. A round of steroids and some anti-inflammatories should have done the trick, but instead there is a fresh new hell to endure. 
Ugh.
If I employ the “coulda/woulda/shoulda” tactic for dealing with the three most-pressing physical challenges, I find myself regretting my decision to put off treatment even though I had met that $6,000 deductible last year. As I face the blank slate of a reset deductible, I wish I’d sucked it up and had the surgeries and procedures I need. Perhaps I would not be typing this very post with pins & needles fingers. Perhaps I would not be thinking about how stiff and sore my knee will be after sitting at my desk to compose a blog post. Perhaps I would not be chiding myself for having been tapped out by the end of 2014.
Cue the mental side of dealing with a physical issue. Because I did not have these problems surgically repaired, I must figure out how to change my thinking. For instance, I give myself a pep talk on the way to the gym. It goes something like this:
“Don’t think about what you used to be able to do, but focus on what you can still do.”
“You’re here.”
“Lots of people more able-bodied than you aren’t even trying.”
“Don’t look at what the other gym-rats are accomplishing; comparison is the thief of joy.”
“Even a shitty workout is better than no workout at all.”
I’m not very good at this part. I recall the words of my favorite yoga teacher: where my mind goes, so too goes my energy. I envision my faulty parts bathed in a warm glow of healing energy. But it’s work. A lot of work. I’m not a fan of listening to my body and accepting limitations; I much prefer to push through the pain. It’s a struggle to avoid falling into the “haven’t I suffered enough??” mentality, and it’s certainly not a great way to start a new year. But, instead of deciding that this old dog can’t learn a new trick, I will become a player (albeit not a starter) in this mental game. As the great Yogi Berra once said, “Ninety percent of this game is half mental.”
The wrong approach?
Posted: August 17, 2014 Filed under: breast cancer, Surgery | Tags: breast cancer in young women, cancer of the nipple, CPM, gut instinct, infectious disease, JP drains, micobacterium fortuitum, Paget Disease, post-mastectomy infection, prophylactic mastectomy 7 CommentsIn this article for The New York Times, Peggy Orenstein addresses one of the many tricky topics surrounding breast cancer: to remove or not remove the “unaffected” breast?
It’s a tricky topic because the research and prevailing medical consensus are in direct opposition to gut instinct. Research says a bilateral mastectomy in patients with cancer in just one breast has little impact on survivability. Doctors say the odds of surviving low-grade noninvasive breast cancer is the same whether we undergo a lumpectomy or a mastectomy. But our guts often say “lop em both off.”
That’s what my gut told me to do, even after extensive research and number-crunching. My gut instinct leaped immediately to a slash-and-burn tactic. My darling breast surgeon required me to wait at least 3 days before making my decision on the lumpectomy vs mastectomy debate; I complied but my decision was made in the first 10 minutes of grasping my diagnosis. My gut told me to opt for the bilateral mastectomy.
I suppose this puts me in the category of women opting for a CPM, or contralateral prophylactic mastectomy. The experts whom Orenstein spoke to about the CPM debate refer to the increase in women undergoing CPM as “epidemic” and “alarming” and believe it is driven by women not fully understanding the math. Girls have always been bad at math, right? That’s the message I got, growing up in the 1970s in suburban America.
A 2013 study done by Boston’s famed Dana-Farber clinic revealed that women younger than 40 with no increased genetic risk who had cancer in one breast believed that “within five years, 10 out of 100 of them would develop it in the other; the actual risk is about 2 to 4 percent.”
Upon my diagnosis, I understood the math. It wasn’t easy and it was confusing. It took time and effort, but it was not beyond me (having a math guru in the house helped tremendously, but the point still stands). I understood that my chances of successfully removing the cancer in my “affected” breast was the same whether it was done via lumpectomy or mastectomy. I understood that my chances of developing the same cancer in the other breast were slim to none, because, as Orenstein says,”cancer doesn’t just leap from breast to breast.” I understood that low-grade noninvasive lazy cancers don’t typically become deadly; it takes a cancer that metastasizes to do that.
I also understood that a bilateral mastectomy is not an easy surgery. Not by a long shot. As Orenstein so colorfully describes it, “breasts don’t just screw off, like jar lids.” Undergoing a mastectomy involves not only losing the breast itself but also (typically) the nipple and areola, as well as the lining of the chest muscles. Factor in the JP drains that are snaked into the traumatized chest, just to add insult to injury. I couldn’t lift my arms for days after my mastectomy and needed help with the simplest things, such as brushing my teeth and applying chapstick. I needed a new, temporary wardrobe of tops that buttoned or zipped up, because lifting my arms over my head to put on or take off a shirt was a no-go for my battered upper body. I needed help — lots of help — which doesn’t jive with my stubborn and independent countenance.
I knew that choosing the harder road of a bilateral mastectomy over the easier, less-invasive lumpectomy did not increase my odds of surviving breast cancer. At least according to the studies. I knew that a mastectomy is much riskier than a lumpectomy. I knew that recovery would be much harder and more time-consuming. Nonetheless, my gut told me to take that more difficult road. My gut was right.
Orenstein spoke to Steven J. Katz, a University of Michigan professor of medicine and health management. He studies medical decision-making, and has found that people tend to react from the gut when confronted with a diagnosis because we are wired to make “fast-flow decisions” that make us want to flee. Understandable to anyone who has been on the other side of the doctor delivering bad news. Upon diagnosis, Orenstein recalls feeling “as if a humongous cockroach had been dropped onto my chest. I could barely contain the urge to bat frantically at my breast screaming, ‘Get it off! Get it off!'” Her version involved a giant cockroach; my version involved a scorched earth.
Dr. Katz says that doctors need to understand how our gut reaction affects our post-diagnosis decision. He speaks of “the power of anticipated regret: how people imagine they’d feel if their illness returned and they had not done ‘everything’ to fight it when they’d had the chance. Patients will go to extremes to restore peace of mind, even undergoing surgery that, paradoxically, won’t change the medical basis for their fear.”
It is a paradox: our intellectual self versus our gut.
Orenstein points out that “it seems almost primal to offer up a healthy breast to fate, as a symbol of our willingness to give all we have to and for our families. It’s hard to imagine, by contrast, that someone with a basal cell carcinoma on one ear would needlessly remove the other one ‘just in case’ or for the sake of symmetry.”
While it may be hard to imagine, there’s no way to predict how one will react to a cancer diagnosis. All the studies and statistics are worthless in the face of the worst-possible scenario, which is facing cancer. I was 40 years old, with 2 kids under the age of 10, when I faced that scenario. Of course I thought of them and the possibility of leaving them motherless and rudderless. Having lost my own sweet mama brought that into even clearer focus. Perhaps my decision to undergo a CPM was based more on emotion than on rational thought. No doubt my gut was driving that bus.
But guess what? My gut is a careful and prescient driver. In steering me toward the more-radical surgery option, my gut saved me. Maybe saved my life, but definitely saved me from undergoing a second mastectomy, one that would most definitely not have been of the CPM variety.
My “unaffected” breast had cancer, too. And Paget disease to boot. Nothing had showed up on any of the myriad tests or scans I’d had before my mastectomy. It was the surgical pathology on the “unaffected” breast that finally revealed those cancers. How long would those cancers have grown, unannounced and unaccounted for, had I not followed my instinct and listened to my gut? I don’t like to think about that.
I’ve learned — the hard way, of course — that I’m one of those medical weirdos whose body does not conform to standard protocols. I’m the kook who gets the weird stuff; to wit, Paget disease accounts for a mere 1 to 4 percent all breast cancers, according to the National Cancer Institute. Ditto the post-mastectomy infection I contracted. Who gets a microbacterium fortitum?? So few people that my infectious disease team — yes, I had a team of ID docs — still wonders where the hell that originated.
We medical weirdos don’t fit into studies or facts or figures. We are the ones who keep their doctors up at night, scratching their heads and wondering what?? what?? what is going on here?? We are the ones for whom the “if it can go wrong, it will” axiom applies. We are the ones who make other people reassess the shittyness of their situation (you’re welcome, by the way).
We are the ones who follow our gut and don’t look back. Is that the wrong approach? Not for me. 
Post-surgery pathology
Posted: July 14, 2014 Filed under: Surgery | Tags: cheers to good news, da Vinci hysterectomy, hysterectomy, pathology diagnosis, post-surgery pathology, salpingo-oophorectomy 9 CommentsIt’s clear.
All clear.
At my one-week post-op visit today, I got a copy of the report and learned a whole bunch of new words: adnexa, fimbriated, myometrial, serosa. Those will come in handy next time I play Scrabble.
My endometrium was described as “tan and lush;” my uterus “tan-pink, smooth, and unremarkable.” I guess when it comes to compliments, the radiologist giveth, and the radiologist taketh away.
That’s ok. Whether tan and lush or unremarkable, those trouble-causing parts & pieces are gone. Good riddance. Cheers to good news and to those three little words: No malignancy identified.
Still an impatient patient
Posted: July 12, 2014 Filed under: Surgery | Tags: breast cancer and young women, Griffin and Sabine, healing after surgery, hysterectomy after breast cancer, impatient patients, Nick Bantock, quotes about patience 4 CommentsI’m a terrible patient.
A very impatient patient.
I’ve written about this topic a time or two. Just the other day, I reported on my status after the summary removal of my last remaining girl parts.
Now, a few days further into the healing process, I feel good but not great. Truth be told, I’d much prefer to see and feel a lot more progress. The days are long when I’m forced to sit and heal. I’d like to say I’m a better patient than I used to be; crikey, I certainly should be given all the practice I’ve had during the last several years. But I’m not. At least not noticeably better.
In “Wisdom from the DL” I labored under the mistaken impression that I was getting better at being a patient:
I’ve been on the DL — disabled list — an awful lot since cancer came to town, and I don’t like it. I don’t like it, but I think I’ve gotten better at it. I’ll never be good at being a spectator in my own life, and I’ll never be one who enjoys the journey in my haste to get to the destination,but I have learned the value of time & place and that sometimes you have to be instead of do. I’ve learned to chant “It’s temporary” a thousand and one times to remind myself that while this is my life, it won’t always be like this.
In “Recovery mode” I was perhaps more realistic and came clean on being a terrible patient:
Recovery is tough, and it’s not one of my favorite things. It’s nowhere to be found on the list of my favorite things. I’m a terrible patient — impatient, restless, and intolerant of my dependent state. However, I’m quite the pro at the recovery process now, after multiple surgeries, and don’t fight it as much as I did in the beginning. I’m not going to win patient of the year award in this lifetime, but I’m not gnashing my teeth over the process this time around. Baby steps.
Here I am again, on the DL and in recovery mode. And I still hate it. I still suck at it. I’m still a very impatient patient.
Amidst a previous recovery–for which surgery, I don’t even recall–I explored some words of wisdom on the topic of patience. A few of my faves:
From Shakespeare’s Othello: “How poor are they that have not patience! What wound did ever heal but by degrees?” By excruciatingly slow degrees, that is.
Alexandre Dumas chimed in: “All human wisdom is summed up in two words — wait and hope.” I’m pretty sucky at both of these.
And from Leo Tolstoy: “The two most powerful warriors are patience and time.” Well, that confirms it: I’m hosed.
Then this from Ben Franklin: “He that can have patience can have what he wants.” Franklin. What a smart ass.
What I want is a time machine. Set to “fast forward” so I can speed through this infernal healing process. Or perhaps a home lobotomy kit, so I can fashion myself a new personality. One marked by patience.
Recovering
Posted: July 10, 2014 Filed under: Surgery | Tags: da Vinci hysterectomy, micobacterium fortuitum, minimally invasive hysterectomy, nosocomial infection, recovering from hysterectomy, young women with cancer 12 CommentsYesterday was my first full day home after my hysterectomy, or The Great Clean-Out, as I like to refer to it. At the risk of jinxing myself, I’ll say I feel pretty good. Real good, considering what went down Monday morning.
In typical fashion, I watched a YouTube video of my surgery after the Clean-Out was complete. It’s fascinating and gross all at the same time. The way the tiny instruments saw away the ligaments connecting the reproductive organs to the body . . . super cool.  It reminded me of “the claw” game at an arcade, but instead of procuring the goodies, “the claw” discards the junk I don’t want anymore. This instrument, about the size of a drinking straw, can chop through body parts and allow them to be removed through a small hole in the belly. Genius. And way better for the patient than conventional, open surgery. Way better, especially, for girls who have lived through a nosocomial infection.
It reminded me of “the claw” game at an arcade, but instead of procuring the goodies, “the claw” discards the junk I don’t want anymore. This instrument, about the size of a drinking straw, can chop through body parts and allow them to be removed through a small hole in the belly. Genius. And way better for the patient than conventional, open surgery. Way better, especially, for girls who have lived through a nosocomial infection.
I’ve got four incisions on my belly: three were for the surgical instruments and one for the camera. I had just woken up yesterday when I snapped this selfie, so the lines traversing my belly are from sleep. 
I felt well enough yesterday to take my dog for a short walk, which we both enjoyed, and I expect we will take another lap today. I sat outside for a while and communed with nature. It was hot, but the sun felt good and the chirping birds and buzzing insects reminded me that life goes on.
My goal yesterday was to avoid taking any narcotics. Check. My goal today is to bathe.
We’re entering into the danger zone of my recovery, in which I feel better and am bored. That’s when I start getting crazy ideas, like “Oh, I’ll just wipe down the kitchen counters.” No. Just no. Step away from the sponge. I’m a terrible patient and am terribly impatient. Yes, I know: there are books to be read, movies to be watched, TV shows to be caught up on, but the days are long and my butt gets numb from so much sitting. So much doing nothing. I really stink at doing nothing.
Perhaps it’s time for some champagne.
Surgery update
Posted: August 23, 2012 Filed under: Surgery | Tags: Bactrim, Elite Surgical Center, knee replacement, knee surgery, lateral release, PRP, Texas Medical Center 18 CommentsThe knee surgery went well yesterday. Got up at the crack of dawn to truck on into the Medical Center and was at the surgery center at 6:10 a.m. Sherpa Amy came prepared with a rollie bag full of projects and snacks, even a picnic lunch. She reminded me to tell the doc that morphine is not my friend via IV but intramuscularly in the behind works fine. She brought me home while Trevor filled my prescriptions, then helped Macy with her knitting. I would love to sing her praises even more but don’t want to risk someone else wanting to partake of her medical concierge services. I’m selfish like that.
After filling out the requisite paperwork, I was escorted back to anesthesia land, one of my favorite places. The anesthesiologist was flat-out awesome. He looked about 25 and played football in college. Based on the size of his thighs, I’m guessing he special-orders his scrubs. He held my hand and said he was taking me to the prom–his little joke to distract me from him inspecting my veins, which are combative and uncooperative on a good day. One quick poke to my left hand, and my prom date was in.
My surgeon came to visit and to double check that I did want the lateral release procedure in addition to the arthroscope. I said yes, please. Ever since I learned that my kneecap was dislocated, I’ve been creeped out and was ready to get it back in line.
After our chat, I got half of my anesthesia cocktail but had to wait for the other half until I got into the OR. I had to haul myself up on the operating table, which would have been difficult if I’d consumed the entire cocktail. I vaguely recall being in the OR but don’t remember getting on the table.
A couple more pics of the lateral release:
Next thing I know, I’m waking up in recovery and fighting hard to keep my eyes open. I’m weird about wanting to prove that I’m ok and ready to go home. Even when I know in my heart of hearts that I should stay, I want to go. Kinda sounds like the basis for a country song. I’ve got an ace bandage from mid-calf to a several inches above my knee, and lord knows what’s under the ace bandage. I’m not all that curious to see. I know that there are 3 incisions, all of which are stitched closed. The ace bandage can come off tomorrow, and I’ll get a look at the stuff inside.
The good news from the surgeon: both procedures were successful. The bad news: I have no cartilage under my knee cap. None. Nada. Zip. So while my kneecap is realigned again, I’ll still be dealing with the pain. Hopefully not as bad as it has been; I’m optimistic, or delusional, either one fits. Dr Alani also said that even after the scope and the lateral release, I can’t do squats or lunges. Ever. Sigh. That makes me quite sad because those are things I actually like to do. I’m weird that way. And stubborn, too: the fact that he says I can’t do it incites me to try. My handlers are going to be hard at work on this one.
Because there’s no cartilage under my kneecap, I will most likely need a knee replacement at some point down the road. Add that to my list of things to do.
Today I have 2 goals: to take my twice-daily antibiotics without letting myself be transported to the awfulness that was 267 straight days of antibiotics after my post-mastectomy infection. I can do this. The second goal is try to bear some weight on my right leg and see how the knee responds. My guess is that its response will be angry. I’m tempted to start weaning myself off the pain meds, but I can hear my handlers protesting that it’s too soon, and that I’m going to need the meds even more after I try to put some weight on my bum leg. But the Lortab makes me itchy and spacey. I can’t take anti-inflammatories because of the PRP he injected into my knee. The autologous injection’s purpose is to stimulate the inflammatory response that helps our bodies heal. Anti-inflammatories short-circuit that response. Same for ice: I’d like nothing more than a big bag of ice on my knee right now, but it too can hinder the PRP’s success. So no ice, no OTC meds for me.
The surgical center staff talked a lot about the pain associated with the lateral release, and I smiled knowingly because I’ve been through so much worse. All I have to do is toss out the words “bilateral mastectomy,” “nosocomial infection,” “multiple tissue debridements,” and “DIEP reconstruction,” and the nurses realized that it’s all relative. An IV in my hand, a few little incisions and some cut connective tissue don’t scare me. Looking back on my previous surgeries reminds me that while it’s a hassle to hobble and a drag to be on crutches, it’s a piece of cake comparatively speaking. If one good thing has come from all the surgeries I’ve had it’s that I’ve learned to be much more patient with the healing process — a big step for a busybody like me. Instead of gnashing my teeth because I’m on the DL again, I’m sending happy, healing thoughts to my beleaguered body. As my sweet survivor sister Jenny reminds me, “It’s temporary.” Hopefully I’ll be recovered in time for some fall tennis, when the sun-soaked TX weather eases a bit.
On this day in history…
Posted: March 2, 2012 Filed under: breast cancer, Surgery | Tags: breast reconstruction surgery, Center for Breast Restoration, DIEP surgery, JP drains, Texas Medical Center, the Big Dig 15 CommentsOne year. 365 days. Or, 366 days with a leap year. Either way, a year is a long time, a lotta days. So much can–and does–happen in the span of a year. Each day is ripe with possibility, and none was as much so as March 2, 2011. Ralph Waldo Emerson once said, “Write it on your heart that every day is the best day in the year.” Looking back at this day last year, I’m taking his advice and am going to write it on my heart: being one year out, exactly, from The Big Dig makes this day the best day in the year. This time last year, I was once again in a hospital gown while my cabal of surgeons brandished multi-colored Sharpies to designate the roadmap that would lead us out of the ravages of infection.
I haven’t yet processed all the thoughts and emotions attached to this day one year ago. I don’t know when or how that will happen. My reconstruction surgery was big. Epic, even. After a long and winding road of “whatever can go wrong did go wrong” post-mastectomy, getting to the point of being able to have reconstruction was major progress. All of the research, doctors’ powwows, appointments, testing, and paperwork involved was just the tip of the iceberg. Then came the actual procedure, and then the recovery. None of those, however, are as arduous as it is to wrap my head around the “journey” that reconstruction was–and still is–for me.
Because I haven’t yet wrapped my head around my reconstruction “journey,” and because frankly I’m kinda scared to pick at that scab and let loose the torrent of emotions lying under the surface, I’m not going to write about it. Yet.
Instead, I present highlights from the surgery day and the days and weeks that followed. As you loyal readers will remember from this time last year, it was several days before I was able to sit at my computer and type. My trusty stand-in bloggers were the hubs, Trevor, and my surgery sherpa and dear friend Amy. They filled in for me when I was unable to process a coherent thought, sit upright, or use my arms.
While I never got bogged down in the “Why me?” school of thought regarding the complications that ensued from my cancer “journey,” I know now that there are a lot of thoughts and feelings still untapped regarding the perilous trek from normal person to breast cancer patient to survivor. So busy was I handling the logistics of each new complication that dealing with the emotional fallout took a backseat to just getting through each new hiccup. I know all you arm-chair psychiatrists out there are shaking your collective heads and tsk-tsking me for tamping down these thoughts and feelings. I would pass the same judgment on any other poor sap in my shoes. However, you do what you gotta do to get through the worst times, and “when you’re going through hell, keep going,” as Mr Churchill so sagely advised.
Mr Churchill would probably also advise me to quit talking about it and get to it, so here, without further ado, are the highlights (or are they lowlights?) of The Big Dig.
After the surgery was finally complete, Trevor was eerily prophetic when he forecasted the tough days ahead: “She is still awake but in a bit of pain. They are not fooling around with it at least and they just upped her pain-med clicker along with a nice big slug of morphine. We have some tough days ahead while she recovers but everything looks great so far.”
After surgery and the recovery room, I was shipped straight to ICU for an unpleasant stay that seemed endless. In Recovery Trevor wrote, “We made it through the first night in ICU. The nurses checked on her every hour last night so she didn’t get too much sleep though. They have ordered a regular room for her but they won’t let her out of ICU until she sits up in a chair for an hour. They just wheeled the chair in, this is gonna hurt.”
I remember how ominous it was when the chair was wheeled into my room. A hush filled the room as everyone realized what was about to take place. Anyone who’s had a C-section knows how difficult it is to move straight after, and with a hip-to-hip incision, “difficult” barely covers it.
Trevor wrote about making the switch from ICU to a regular hospital room: “Finally out of ICU. It took forever to get out of there, there just seemed to be always one more thing. They had to take blood and couldn’t get enough from the line in her hand despite much digging and infliction of pain. They finally just opened up her chemo port and had it done in a snap. Of course they had already packed her up for transport so the morphine pump was temporarily disconnected. But Nancy is a bad ass and toughed it out.”
I have no recollection of this at all. That’s probably a good thing. I’m glad I was a bad-ass about it, though.
In So Long ICU Amy wrote: “She’s super tired. Come to find out her new breasticles have to have their arterial blood flow checked once an hour and it’s been that way since the surgery ended yesterday and will be through tomorrow…..so cat naps abound. They made her get up and have a ‘sitting trial’ time for an hour and she did really well. To hear her tell the doctors about it, it was ‘hard’ but as an observer she handled the “trial” with grit and humor–typical Nancy. Tomorrow’s plan is to do a little bit of walking and take a shower.”
It wasn’t long before the wailing & gnashing of teeth commenced. As soon as I made the transition from drugged up to mildly lucid, I figured out that this wasn’t going to be an easy recovery. In Utter Exhaustion Amy explained: “I’ve only had to charge her the $10 for ‘having to put up with your complaints fee’ twice today. As much as Nancy would like you to think she’s a troublesome patient, she is not, at all. In fact, the staff enjoy her very much. Her easygoing nature was complimented today when she had to make the effort to get in the chair to sit for another hour. Le, her nurse, commented about how Nancy’s attitude really made her job easier.”
I put on a happy face for my medical peeps, but was a bit more realistic with my closest caregivers.
Amy continues: “Complaint number 1: This particular complaint is what brought on the $10 charge twice today. The ICU room was hot, very hot. In fact there were heaters brought in just for this purpose…two of them. Seems that the stomach tissue that they harvested for her new rack doesn’t realize that it has to get its heat source from her body instead of the outside air, so for the next few weeks Nancy needs to have a warmer than normal outside air temperature. I think the docs even suggested turning off the AC at her house once she gets out of here, but Nancy and I decided to let that one go over our heads. Nancy actually assessed herself the charge after I mentioned that I charge $10 at my house for being ‘grouchy, irritable, or just plain mean.’ Then she said, ‘And you can charge me another $10 for this one…..’ Complaint number 2: Headache. A bad one. She’s been dealing with this all day. The nurses say she had a pretty major dose of morphine in the ICU so that is a side effect of morphine and it should work itself out as she uses less and less morphine. Because of this, Nancy has decided that Mr. Morphine Pump may not be summoned every time the pain surges. She’s thinking about it before she presses the button. On one side there’s the headaches. On the other side there’s the pain. It’s a delicate seesaw to manage.”
“The good news is that despite the pain, she managed to move from her bed to the recliner, sat for an hour, then ambulated back to the bed with only 1 morphine pump at the beginning of the whole scenario. The nurses are impressed with how tough our girl is!”
I still owe Amy $20. Maybe more.
My intrepid sherpa wrote the Morning Report the day after I was released from ICU: “This morning the muscle tightness and tenderness in the belly incision reared its ugly head and has taken the forefront in the battle for attention. While Nancy hasn’t actually called it pain, I think that may be the best word for it. There’s a lot of bruising around the hip-to-hip incision, and the docs said that they did had to work hard with her muscle layer there as well as on her chest wall so this is to be expected. She has been given Flexeril (a muscle relaxer) to help with this and the added benefit is that it makes her VEEEERRRYYY sleepy. So, even though at 5:15 AM, Nancy was confident that she was up for the day and we did the teeth brushing and face washing that comes with a new day, she was within minutes back to sawing logs. Good Girl! She has been dreaming out loud and woke asking me, ‘Is that due tomorrow?’ You can take the Mom out of the home but you can’t take the Home out of the Mom!”
Whatever assignment was due hopefully got done; I have no idea what it was!
Rejuvenated?? was written 2 days after surgery, by Amy: “Mr. Morphine Pump and the rest of his crew are yet again dust in the wind. Nancy is free of anything that follows her on a pole. She does have 6 drains and 2 doppler wires, plus her central line access port, so she’s still got a little gear. The big event today was a shower. Well, all I have good to say about that shower is that Nancy is clean. One word I could use to describe how Nancy tolerated the event was that she was speechless. So, suffice it to say that the pain from the ab incision reached out and grabbed hold of her. By the time she had recovered enough from the trauma of the shower to find her voice she said, ‘That’s NOT happening again! I’m clean enough!'”
Finally, I was able to post for myself and in 1 Week Ago, I got to it: Long story short, the flaps [newly fashioned breasts from belly tissue] were cooperating, the morphine headache abated, some regular food arrived, and life rolled on. At some point they moved the flap checks to every two hours instead of hourly, which was mighty nice. It’s amazing how your perspective changes in a situation like that. After umpteen hours with no food, a simple PB&J was a delicacy. After being awake most of the night, a short cat-nap seemed a decadent luxury. While I feel a whole lot better and am ready to get back to normal, my handlers think one week post-op is a bit premature to jump right back into the day-in, day-out routine. I am trying to take it easy. I’m resigned to the fact that I’m back to one outing a day for a while, and sadly, a doctor’s appointment counts as an outing. Yesterday I had a small entourage escort me to for my checkup, and we had a bite of lunch (sans margaritas) beforehand.  The handlers insisted on snapping a photo of this maiden voyage, and there was some talk of me earning a margarita for every device I had removed at the subsequent appointment. Between the two doppler wires and the 4 JP drains, somebody owes me 6 margaritas. No salt.”
The handlers insisted on snapping a photo of this maiden voyage, and there was some talk of me earning a margarita for every device I had removed at the subsequent appointment. Between the two doppler wires and the 4 JP drains, somebody owes me 6 margaritas. No salt.” 
A little later, in Wisdom from the DL, I got real about my hatred of all things invalid-related: “I’ll never be good at being a spectator in my own life, and I’ll never be one who enjoys the journey in my haste to get to the destination,but I have learned the value of time & place and that sometimes you have to be instead of do. I’ve learned to chant It’s temporary a thousand and one times to remind myself that while this is my life, it won’t always be like this.”
One year later–one very long year that was equally horrific and hard yet insightful and triumphant–I’m still reminding myself.











