The wrong approach?
Posted: August 17, 2014 Filed under: breast cancer, Surgery | Tags: breast cancer in young women, cancer of the nipple, CPM, gut instinct, infectious disease, JP drains, micobacterium fortuitum, Paget Disease, post-mastectomy infection, prophylactic mastectomy 7 CommentsIn this article for The New York Times, Peggy Orenstein addresses one of the many tricky topics surrounding breast cancer: to remove or not remove the “unaffected” breast?
It’s a tricky topic because the research and prevailing medical consensus are in direct opposition to gut instinct. Research says a bilateral mastectomy in patients with cancer in just one breast has little impact on survivability. Doctors say the odds of surviving low-grade noninvasive breast cancer is the same whether we undergo a lumpectomy or a mastectomy. But our guts often say “lop em both off.”
That’s what my gut told me to do, even after extensive research and number-crunching. My gut instinct leaped immediately to a slash-and-burn tactic. My darling breast surgeon required me to wait at least 3 days before making my decision on the lumpectomy vs mastectomy debate; I complied but my decision was made in the first 10 minutes of grasping my diagnosis. My gut told me to opt for the bilateral mastectomy.
I suppose this puts me in the category of women opting for a CPM, or contralateral prophylactic mastectomy. The experts whom Orenstein spoke to about the CPM debate refer to the increase in women undergoing CPM as “epidemic” and “alarming” and believe it is driven by women not fully understanding the math. Girls have always been bad at math, right? That’s the message I got, growing up in the 1970s in suburban America.
A 2013 study done by Boston’s famed Dana-Farber clinic revealed that women younger than 40 with no increased genetic risk who had cancer in one breast believed that “within five years, 10 out of 100 of them would develop it in the other; the actual risk is about 2 to 4 percent.”
Upon my diagnosis, I understood the math. It wasn’t easy and it was confusing. It took time and effort, but it was not beyond me (having a math guru in the house helped tremendously, but the point still stands). I understood that my chances of successfully removing the cancer in my “affected” breast was the same whether it was done via lumpectomy or mastectomy. I understood that my chances of developing the same cancer in the other breast were slim to none, because, as Orenstein says,”cancer doesn’t just leap from breast to breast.” I understood that low-grade noninvasive lazy cancers don’t typically become deadly; it takes a cancer that metastasizes to do that.
I also understood that a bilateral mastectomy is not an easy surgery. Not by a long shot. As Orenstein so colorfully describes it, “breasts don’t just screw off, like jar lids.” Undergoing a mastectomy involves not only losing the breast itself but also (typically) the nipple and areola, as well as the lining of the chest muscles. Factor in the JP drains that are snaked into the traumatized chest, just to add insult to injury. I couldn’t lift my arms for days after my mastectomy and needed help with the simplest things, such as brushing my teeth and applying chapstick. I needed a new, temporary wardrobe of tops that buttoned or zipped up, because lifting my arms over my head to put on or take off a shirt was a no-go for my battered upper body. I needed help — lots of help — which doesn’t jive with my stubborn and independent countenance.
I knew that choosing the harder road of a bilateral mastectomy over the easier, less-invasive lumpectomy did not increase my odds of surviving breast cancer. At least according to the studies. I knew that a mastectomy is much riskier than a lumpectomy. I knew that recovery would be much harder and more time-consuming. Nonetheless, my gut told me to take that more difficult road. My gut was right.
Orenstein spoke to Steven J. Katz, a University of Michigan professor of medicine and health management. He studies medical decision-making, and has found that people tend to react from the gut when confronted with a diagnosis because we are wired to make “fast-flow decisions” that make us want to flee. Understandable to anyone who has been on the other side of the doctor delivering bad news. Upon diagnosis, Orenstein recalls feeling “as if a humongous cockroach had been dropped onto my chest. I could barely contain the urge to bat frantically at my breast screaming, ‘Get it off! Get it off!'” Her version involved a giant cockroach; my version involved a scorched earth.
Dr. Katz says that doctors need to understand how our gut reaction affects our post-diagnosis decision. He speaks of “the power of anticipated regret: how people imagine they’d feel if their illness returned and they had not done ‘everything’ to fight it when they’d had the chance. Patients will go to extremes to restore peace of mind, even undergoing surgery that, paradoxically, won’t change the medical basis for their fear.”
It is a paradox: our intellectual self versus our gut.
Orenstein points out that “it seems almost primal to offer up a healthy breast to fate, as a symbol of our willingness to give all we have to and for our families. It’s hard to imagine, by contrast, that someone with a basal cell carcinoma on one ear would needlessly remove the other one ‘just in case’ or for the sake of symmetry.”
While it may be hard to imagine, there’s no way to predict how one will react to a cancer diagnosis. All the studies and statistics are worthless in the face of the worst-possible scenario, which is facing cancer. I was 40 years old, with 2 kids under the age of 10, when I faced that scenario. Of course I thought of them and the possibility of leaving them motherless and rudderless. Having lost my own sweet mama brought that into even clearer focus. Perhaps my decision to undergo a CPM was based more on emotion than on rational thought. No doubt my gut was driving that bus.
But guess what? My gut is a careful and prescient driver. In steering me toward the more-radical surgery option, my gut saved me. Maybe saved my life, but definitely saved me from undergoing a second mastectomy, one that would most definitely not have been of the CPM variety.
My “unaffected” breast had cancer, too. And Paget disease to boot. Nothing had showed up on any of the myriad tests or scans I’d had before my mastectomy. It was the surgical pathology on the “unaffected” breast that finally revealed those cancers. How long would those cancers have grown, unannounced and unaccounted for, had I not followed my instinct and listened to my gut? I don’t like to think about that.
I’ve learned — the hard way, of course — that I’m one of those medical weirdos whose body does not conform to standard protocols. I’m the kook who gets the weird stuff; to wit, Paget disease accounts for a mere 1 to 4 percent all breast cancers, according to the National Cancer Institute. Ditto the post-mastectomy infection I contracted. Who gets a microbacterium fortitum?? So few people that my infectious disease team — yes, I had a team of ID docs — still wonders where the hell that originated.
We medical weirdos don’t fit into studies or facts or figures. We are the ones who keep their doctors up at night, scratching their heads and wondering what?? what?? what is going on here?? We are the ones for whom the “if it can go wrong, it will” axiom applies. We are the ones who make other people reassess the shittyness of their situation (you’re welcome, by the way).
We are the ones who follow our gut and don’t look back. Is that the wrong approach? Not for me. 
Fever-free, finally?
Posted: August 31, 2011 Filed under: breast cancer, cancer fatigue, drugs, infection | Tags: Houston medical center, infectious disease, long-term antibiotics, Maria Pace-Wynters, post-mastectomy infection, psychological effects of breast cancer 7 CommentsYesterday was the first day since my surgery–exactly one week ago–that I didn’t have a fever for most of the day. I wasn’t exactly fever-free, as my temp peaked at bedtime, but that’s the best it’s been for one very long week, so I’m claiming it. After coming this close to needing IV antibiotics — again — I’m beyond thrilled to have been (mostly) fever-free yesterday. I’m guessing that the docs in my life would laugh a little, shake their heads, and maybe massage their temples a bit at me claiming yesterday as fever-free. I’m guessing my friends in the white coats would consider my being almost fever-free akin to being a little bit pregnant–it’s an all-or-nothing condition. That’s fine. They can chuckle and shake their heads at me, I’m still claiming it as a victory.
See, fever can indicate infection, and after my surgery last week, the fear of recurrent or new infection abounded. That fear was thick in the OR and it was pervasive in the days after surgery as we waited to see what would happen. It’s still lingering, in the back of my mind and on the fringes of my daily activities. I’m not a big fan of that loss of control. We did increase my course of oral antibiotics — both in duration of course and milligrams per dose. The usual suspects in the roster of awful side effects are back, but that tells me the abx are working. If there was a niggling infection trying to re-establish itself, the mounds of abx I’ve been taking for the last 7 days have contained it. I’m almost afraid to say this out loud, but I think I’m out of the woods.
Can it be? Like the joyous girl in the gorgeous Maria Pace-Wynters art, coincidentally titled “Out of the Woods,” I want to smile big and enjoy the view of the woods from the other side. I want to feel the relief that washes over me as I realize that the 6-day fever has broken, the pain & redness & swelling in the original infection site have abated, and I may be able to breathe easily now.
My infection-induced PTSD makes me wonder if I really can believe that the tide is turning, that I may be out of the woods. It’s been a long, long haul. A super-long haul. Reflecting back on the havoc that the post-mastectomy infection has wrought makes me very uncomfortable. I’m not yet in that happy place, and the calamity is not far enough in the rear-view mirror yet. Instead of feeling enormous pride, accomplishment, gratitude and general kick-ass-itude that it’s over, I’m gun-shy and untrusting.
This time last year, I was fresh out of the hospital, having just served day 27 of intermittent, back & forth hospital stays and at-home IV antibiotics. The last hospital stay to treat the infection was at Methodist in the Med Center, so I’d served time in 3 different hospitals–Memorial Hermann Southwest, Methodist Sugar Land, and Methodist Med Center–which allowed me to sample Houston’s best. I recall the direct-admit to the Med Center for the last stay, late on a Sunday night just before school started. Sweet Dr S had handled the details for me so I had a “fast pass” to get admitted quick, which allowed me to circumvent the circus that is a Med Center ER on a weekend night. Dr S and I were texting back & forth during the speedier-yet-still-complicated process so he would know that I was in the room before he had to get up and leave his family to come see me and get all of our ducks in a row.
I remember being furious about having to go back into the hospital. At that point last year, I’d been on antibiotics all summer, oral and IV, in every imaginable combination. Biaxin. Cipro. Minocycline. Zyvox. Vancomycin. Cefapim. Doxcycline. Bactrim.Vancanese. Levaquin. We were on the cusp of finding the magic bullets that would target the slow-growing and slow-to-kill infection (Bactrim & Minocycline), but it would take time to decimate the wily bacteria, so the infection still had the upper hand. As I settled into my room after navigating the maze that is Methodist Med Center, I was completely and utterly pissed at the ugly-ass artwork in my room. The shoddy impressionist landscape was hideous, the colors were barf-inducing, and the mere site of it reminded me that I was once again a prisoner — of my failing body and of yet another hospital. I couldn’t avoid that uproariously unpleasing “artwork” because it was in my face and I had nowhere to go to avoid it. That framed print became a symbol, a poster-child if you will, for all that had gone wrong last summer, and I was stuck staring at it. If I hadn’t been so ticked and so upset, I would have taken a picture of that “artwork,” and one day it will make me laugh instead of making me want to punch someone. But not yet.
Here’s what I wrote upon settling into that room; note the frustration surrounding the words that described the room but actually meant a whole lot more:
So I got through the masses in the ER pretty quickly and got into my room and thought, yuck, this place is a dump compared to my lovely one-bedroom suite at Methodist Sugar Land. Call me a snob, but I like those hardwood floors and new, unchipped paint. I don’t really need the laminated sign on the wall here reminding me not to leave my dentures on my lunch tray. The view out my dirty window is of a wall, with patient rooms too far away to spy into [one of my pastimes at Methodist Sugar Land]. The chair I’m sitting in to type this is vinyl, and there is a lovely faux-cherry-wood desk with ornate colonial drawer pulls. I could sit there, but the desk chair is super scratched with dingy upholstery on the seat cover. And don’t even get me started on the artwork on the wall across from the 20-year-old bed covered in ultra-scratchy sheets. No wonder people get sick in hospitals. It’s from the decor as much as the bacteria.
I was one unhappy girl.
I was coming to terms with the fact that the infection superseded the cancer in every way. For a while, that was a good thing — being so focused on the infection kept me from thinking about the fact that I was a 41-year-old mother of 2 young kids battling cancer. The cancer was easy compared to the infection. While a cancer diagnosis is one of the scariest things ever, the treatment for and eradication of that cancer was, for me, much more logical and linear than the infection. The cancer left me flat-chested, but once the tumors were removed and the lymph nodes declared clear, it was done. My game plan was defined: a 5-year course of Tamoxifen for adjuvant therapy along with hormone suppression to snuff the cancer’s fuel. The cancer battle was over and the treatment had begun, but the infection war hadn’t even revved up yet. Little did I know that more than a year later, I’d still be fighting that war, and that sometimes the infection would gain ground and force me to retreat.
The infection left me with a hole in my newly flat chest — literally. The excised tissue created a wound that measured 5.6 cm long and 3 cm wide. Grab yourself a ruler and feast your eyes on those dimensions. That bad boy took 8 weeks to heal, almost double the healing time required by my bilateral mastectomy. I’d faced my diagnosis, done my research, made the hard decisions, endured the systematic removal of both breasts, and was still standing. The infection, however, was a whole ‘nother ball game. There was no logic and nothing was linear — it was a guessing game. Educated guesses by a crack team of infectious disease docs, but a guessing game nonetheless. Will this combo of antibiotics work? How long will I need to stay on them? How will we know if they’re working? What are the side-effects of long-term abx therapy? Will I ever get my normal life back? The questions were many, the answers were few. I wrote this after one particularly frustrating day in the infection war:
All this talk you hear about being a pro-active patient, being your own advocate, researching and digging up as much info as you can and thinking for yourself — forget it. Today is one of those days that makes me wish I was a sheep. I just want to follow along and do what I was told. Except I can’t. It’s not how I’m made. So I continue to ask questions and solicit advice, all the while feeling like I don’t have all the puzzle pieces. Sometimes there are a few pieces missing, or you have to wait a while for them to fall into place. You can’t force it, although I want to. I am impatient and a forcer. An impatient forcer.
And I’m still waiting for the pieces to fall into place.
Meanwhile, I will feast my eyes on another gorgeous piece from Maria Pace-Wynters’s collection. This one is titled “Unseen Beauty,” and my eyes are open. 
No autographs, please
Posted: July 11, 2011 Filed under: baseball, breast cancer, infection | Tags: baseball, breast cancer, cancer battle, First Colony Little League, hospital, infection, infectious disease, IV antibiotics, Little League All Stars, mastectomy, post-mastectomy, psychological effects of cancer, recovery, summer camp, Vancomycin 4 CommentsToday is a very good day, for 3 reasons, maybe more. #1: Macy started two weeks of Fine Arts camp, which she loves (and I’m rather fond of having a few hours to myself while she’s off doing fun projects that someone else cleans up, and by “someone else” I mean anyone but me). While she hasn’t gotten quite this messy in a while, she’s definitely still got it in ‘er. 
#2: I did push-ups at the gym this morning. It’s been a long time since I’ve been able to do them, and there’s a bit of pride on the line since I was working out with my 12-year-old son. I wasn’t about to let him see me doing “girlie” push-ups with bent knees, so I tried the real thing, and while it didn’t feel great, I did it. Pre-cancer, pre-mastectomy, and pre-infection, I used to be able to do 50 push-ups like it was nothing, and while I’m not there yet, I’m getting closer.
#3: The article for which Payton and I were interviewed was published in our community newspaper. Corey the reporter was nice, and I think he’s a good writer. He has covered the district All Star games for all the ages, and he’s made the games come alive in his stories. P really enjoyed being interviewed; I like the drama of the article, especially the part in which I’m portrayed as “fighting for my life” (cue the dramatic music here).
It’s a good reminder to be careful what you say, too, because I joked with Corey about P having gotten his mad baseball skills from my side of the family. While it’s true–my dad’s baseball career started with PeeWee ball in 1948 and ended with him playing for the University of Tulsa–I was being smart-aleky, and Corey not only took it seriously but also included that in the article! I certainly don’t want to sound like one of “those” baseball moms. I think my kid is a good player who happens to have some natural athletic ability and a body built for taking some hard knocks. However, I’m under no illusion that he’s going to play ball for a living when he grows up, and his *$#& most definitely stinks.
While I can take or leave the publicity, reading the latest article did make me realize that a whole lot has changed since this time last year. And most of that change has been good. Really good.
This time last year, Payton’s All Star team was preparing for the sectional tournament, which they totally dominated, BTW. But I was fighting another battle against that damned nosocomial infection and was back in the hospital. Again. So after P’s team swept the sectional tourney, they were preparing to go to the State Championship in the lovely Tyler, TX. I remember thinking on that Monday, the day I was admitted to the hospital–again–that we’d get the infection under control, pump in some more vancomycin and I’d be on my way to Tyler.
Yes, I was that delusional.
Instead of the scenario playing out the way I’d envisioned, it went something like this: I was admitted on a Monday and didn’t get out until Thursday. An area that started as a red, streaky site on the mastectomied right chest wall had to be opened up, drained, excised, and packed with gauze. Repeatedly. The packing part was particularly brutal. See, there was a bunch of fluid inside my chest wall from the infection. Dr S cut a track–sans anesthesia, I recall–to open and elongate the drain hole, to let the fluid out. Once the track was there, though, it had to be packed with gauze to soak up all the nasty fluid. It wasn’t a quick process, because the hole and the track were small but had to be completely filled with gauze, for maximum soaking. Thus, a lot of shoving in an already sore, infected, and aggravated area was required. As was a lot of xanax. At one point, after Dr S shoved the gauze into the open wound, my blood pressure was 212/65. That’s a little high for me.
I survived 4 days of intense wound-packing and hard-core IV antibiotics. But just barely. I missed the entire State Championship experience, then put my kids on a plane for summer vacation, that I didn’t get to attend. I did manage to stay out of the hospital for 2 and a half weeks, but had IV antibiotics at home and a home health care nurse packing that wound. I was hoping to have turned a corner after all that (and more than once wondered what it would take to finally kick that infection) but was back in the hospital again the week before school started.
It was not a good summer, to say the least. This one has been much, much better. While the bar wasn’t exactly set very high after last summer, this one is pretty sweet.
A whole new ball game
Posted: June 30, 2011 Filed under: baseball, breast cancer | Tags: All Stars, baseball, cancer and young kids, cancer battle, First Colony Little League, hospital, infection, infectious disease, Ipad apps, Little League, moms with cancer, post-mastectomy, psychological effects of cancer, recovery, Salisbury Beach, West University Houston 9 CommentsI’m as nervous as a cat. On a hot tin roof.
Payton’s All Star team was one game away from being district champions last night, and they went down in flames. We’d already beaten the West University team but they came back with a vengeance (and their best pitcher). As a seasoned baseball mom who’s used to watching a confident & uber-talented team, I can usually get a read on the game and have a sense of how it’s going to end. Last night I didn’t have my usual “sixth sense” before the game, and even when our boys launched 2 homers in their first at-bat to take a 3-0 lead, I didn’t settle in with my usual feel-good feeling about the outcome.
My kid got hit by a pitch during his first at-bat. Not a wimpy pitch, either, but a smokin’ fastball. That fastball thumped his thigh, just above the knee, quite audibly. My mama- bear instinct kicked in and I was on my feet, wondering if my boy would crumple in a heap on top of home plate. Then my rational brain kicked in and reminded me that my boy is tough as nails and meaner than a red hog on the field. He takes pain like it’s a cool summer breeze, as if it’s a “woonty” on the shore of Salisbury Beach. His pain tolerance is incredible, and yes, he gets that from me. He’s the ideal football player — a coach’s dream — because he’d rather take a beating than admit he’s hurt. Most kids take a “test jog” down the right-field line after being hit by a pitch, to make sure they can still run without a hitch in their giddy-up. Not my kid. After being pounded, my kid just casually tossed his bat and trotted to first base. Not a wince or a whimper from him.
Here’s the after-effect. I expect it to become much more colorful in the coming days. 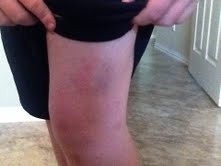
Payton’s teammate Gus responded to the bean-ball by hitting a homer off the pitcher who pegged my kid. Way to go, Gus!
Sadly, the First Colony bats weren’t as hot for the rest of the game, and we came up short. Errors in the field added insult to injury, and the boys in red got a long, stern talking-to from their coaches instead of a celebratory toast at the local pizza joint.
We face West U again tonight, and will likely bring a renewed vigor for victory. It’s winner take all tonight, so the stakes are high. Whichever team goes home tonight with a victory moves on to the sectional tournament, with hopes of progressing through that and onto the State Championship. Last year, that team was ours, and we’re all hoping for a repeat performance.
No one wants this more than me, since I missed every bit of it last summer. Thanks to a post-mastectomy infection, I was in the hospital instead of in the stands. The team honored me by wearing pink sweatbands throughout the summer, and Payton still wears his.  We had to get a new pair, though, because the original pair was filthy. The kind of filth that repeated washings and soakings and pre-treating can’t remove. Lots of sweat but no tears last summer.
We had to get a new pair, though, because the original pair was filthy. The kind of filth that repeated washings and soakings and pre-treating can’t remove. Lots of sweat but no tears last summer.
Apparently I’m a bit nervous , as I was awake at 4:20 a.m. thinking about tonight’s game. Someone asked me at the gym the other day if I’m one of “those baseball moms.” I wasn’t sure what she meant — the kind of baseball mom who attends all the games and cheers for everyone on the team? Or the kind of baseball mom who gripes at the coach and yells at the umpire about being unfair toward her baby? I’ve seen both kinds. I like to think of myself as the former, but I have been known to yell at an ump a time or two over a particularly egregious call. I am the kind of baseball mom who wears my kid’s jersey to the games, proudly displaying #11 on my back just as my kid does. I am the kind of baseball mom who decorates the car windows, as is tradition around here, so that everyone on the road and in the parking lot know that there’s an All Star on board. 
I am the kind of baseball mom who feels deep pride at my kid being selected for All Stars. 20 players are chosen, then that group is whittled down to 11 or 12 for the traveling team. Lots of players — and lots of moms — would give their eye teeth to be a part of this team. Missing the games and the camaraderie last summer was hard. Really hard.  I was able to follow along with the games via an iPad app that allows a user at the game to enter the pitch-by-pitch action so a user on the other end can follow the play-by-play. One of the moms asked me last night if it’s more nerve-wracking to follow along or to watch the game live. I said watching live is way more nerve-wracking. Sitting in a hospital bed staring at the iPad screen isn’t nearly as complete an experience as being in the stands, in the heat, with the roar of the crowd and the sounds of the game. I do have fond memories, though, of the nurses who were constantly in and out of my room getting involved and asking for updates on the game. And I distinctly remember forgoing pain medicine so I could be lucid enough to follow the game. This summer is a whole new ball game, for me.
I was able to follow along with the games via an iPad app that allows a user at the game to enter the pitch-by-pitch action so a user on the other end can follow the play-by-play. One of the moms asked me last night if it’s more nerve-wracking to follow along or to watch the game live. I said watching live is way more nerve-wracking. Sitting in a hospital bed staring at the iPad screen isn’t nearly as complete an experience as being in the stands, in the heat, with the roar of the crowd and the sounds of the game. I do have fond memories, though, of the nurses who were constantly in and out of my room getting involved and asking for updates on the game. And I distinctly remember forgoing pain medicine so I could be lucid enough to follow the game. This summer is a whole new ball game, for me.
girls’ trip
Posted: June 22, 2011 Filed under: breast cancer | Tags: breast cancer, cancer battle, cancer diagnosis, Fuqua School of Business, hospital, Houston, infection, infectious disease, IV antibiotics, MBAs, mycobacterium, older grad students, post-mastectomy, PTSD, recovery, South Padre Island, survivor, top-10 business school 8 CommentsOnce upon a time, in a city far, far from Houston, there was a group of young-ish women. All had relocated from every corner of the country with young kids in tow to help fulfill their husbands’ dream of getting an MBA from a top-10 business school.
 None of the women knew anyone in the new city, and all were a long way from home. For two long years, without paychecks and luxuries like babysitters, the women bonded while the hubs crammed their brains with all things MBA-related. Once the menfolk had diplomas in hand, the group of women dispersed, to new homes in new corners of the country.
None of the women knew anyone in the new city, and all were a long way from home. For two long years, without paychecks and luxuries like babysitters, the women bonded while the hubs crammed their brains with all things MBA-related. Once the menfolk had diplomas in hand, the group of women dispersed, to new homes in new corners of the country. One night before going separate ways, the women left the hubs and kids at home and went out for a nice dinner. There the plans were laid and a vow was made: let neither distance nor the rigors of child-rearing sever the bond created by hardship and the shared need for breaks from their preschoolers. The solution: come together for an annual girls’ trip, to reconnect and recharge.
One night before going separate ways, the women left the hubs and kids at home and went out for a nice dinner. There the plans were laid and a vow was made: let neither distance nor the rigors of child-rearing sever the bond created by hardship and the shared need for breaks from their preschoolers. The solution: come together for an annual girls’ trip, to reconnect and recharge. 
The first trip was to San Francisco, then Sanibel Island in Florida. Next came Captiva Island, then Scottsdale. Park City was next, followed by Lake Tahoe. Every year was a different locale, but the theme was the same: reconnecting. 
The women had gone their separate ways, and a few left the domestic scene to pursue careers in law and medicine. The others continued to toil on the homefront, trading preschool and playdates for elementary school and homework. The kids grew up, and a few new babies joined the fold. One thing remained the same, however: the women’s commitment to the annual trip.
The End
Well, not really the end. Just the end of my little story.
It’s the eve of the 7th annual Duke girls’ trip, and my suitcase is packed. My boarding pass is printed. My Kindle is full of new books to be read uninterrupted by young children. My house is stocked for my peeps to exist in relative ease in my absence. I’m going, I’m really going.
After 7 years, you’d think that preparations for the trip would be somewhat by rote. Decide on the locale, find lodging, book flights, pack a bag, kiss the fam good-bye, and vamoose.
But not for me. See, last year I was ready for Tahoe. That trip was to have taken place 4 weeks post-mastectomy. As I described it this time last year, the trip was “my goal, a partial finish-line, and my sanity-saver since my diagnosis.” One of the first things I asked my superstar breast surgeon, Dr Dempsey, upon diagnosis, was if I’d still be able to take my girls’ trip. Tahoe with my Duke girls gave me something concrete to work toward in my recovery from surgery, from being diagnosed with cancer at age 40.
Instead of stocking the fridge and packing my bags this time last year, I was in the hospital, sick–really sick–with a nasty infection. I was admitted to the hospital unexpectedly when symptoms of the infection appeared out of nowhere. I literally had seen Dr S the day before the symptoms cropped up; fine one day, sick the next. The day I was hospitalized, I was still clinging to the hope that I’d be in & out of there quickly and still be able to go on my trip. Silly, silly girl. My mind was willing, but my body said “No can do.”
After countless IV bags full of different antibiotics, my fever kept spiking and I got worse instead of better. While the scarier bugs like anthrax were quickly ruled out, the specific infection remained elusive. My infectious disease doc told me that the cultures grow at their own pace, and the culturing is done old-school: in a Petrie dish in an incubator in the lab downstairs. I was confined to the hospital bed until the growth was complete, and no one knew when that would occur. The day before the Tahoe trip, I had to concede that I wasn’t going to make it. Rotten luck.
While it broke my heart and seriously injured my fighting spirit to tell my Duke girls I wouldn’t be joining them, untold hard times followed. Missing the trip was chump changed compared to what was to come. Looking back at my Caring Bridge journal entry for June 10th of last year yielded this:
“I should be on a plane right now, en route to Tahoe, but instead I’m in an ugly gown, sitting on scratchy sheets in an uncomfortable bed (most definitely not a Tempurpedic mattress). Looks like I’ll be here a while yet.”
I don’t recall this part, but it must have happened:
“They moved me across the hall last night to a new room. My new neighbor is an older Asian man who talks louder than anyone I know, and so do all of his relatives. In fact, I just got up my scratchy sheets & walked across the hall in my ugly gown to shut his door. Sheesh. This hospital has an entire floor for Asian patients, which is pretty cool and indicative of this huge city we live in, but I’m wondering why he’s not on that floor.”
Tonight, on the eve of the 7th annual Duke girls’ trip, there are no scratchy sheets and there is no ugly gown. There’s a not-so-youngish-anymore woman who’s had one helluva year, who’s ready to get on that plane and make up for lost time. SPI, here I come. Now that’s a happy ending!
At the ballpark, again
Posted: June 22, 2011 Filed under: baseball, breast cancer | Tags: baseball, breast cancer, cancer battle, cancer diagnosis, family, First Colony All Stars, gratitude after cancer, hospital, infection, infectious disease, life after cancer, Little League, mycobacterium, nosocomial infection, post-mastectomy infection, psychological effects of cancer, survivor, young kids and cancer 5 CommentsLast summer was pretty bad for me and my family. It started innocently enough, with a bilateral mastectomy at age 40 on May 13th, and while I healed quickly and nicely from that, it all went downhill fast.
Just after my 41st birthday, I got a nasty post-surgery infection. No one saw it coming, and to say it took us all by surprise would be a gross understatement. The odds of contracting a nosocomial infection are not small, but my infection is somewhat rare, quite wily, and super slow to treat. In the scope of inconvenient infections, I won the lottery.
Last night was the first game of the All Star tournament for Payton’s team–something I missed entirely last summer. Being present last night to watch my boy do what he does best with his team of like-minded and uber-talented buddies was one of the simplest yet deepest thrills of all time. We take a lot of things for granted in this life of ours, and being able to sit on metal bleachers in the Texas heat in June to watch youth baseball is one of those things. I’ve sat through thousands of games for my little ball player, and hardly thought twice about it beyond the random, mundane thoughts associated with this endeavor: who are we “versing” (as our catcher, #10 Carl says)? Where is Payton in the line-up? Are we on the shady side of the field? Did I remember my stadium seat? How many times will Macy hit the concession stand? How many pieces of bubble gum does Pay have in his mouth at once?
Those are the thoughts that traverse my brain during a game, along with the usual baseball stuff: What’s the run rule in this tournament?; How did we fare against this team last time we met? If the ball hits the bat then hits the batter, he’s out, right? Rules and regulations course through my head as I follow the many games my boy has played.
Last night was different, though. As I was ready to walk out the door, our bestie Ed reminded me that I’ve come a long way since this time last year. Several of the parents on our team remarked at the park that it’s nice to have me there this year. A couple of the coaches said something about having missed me and my big mouth last summer; once a cheerleader, always a cheerleader.
I have come a long way since last summer, and watching my kid play ball is something to be savored, something to most definitely not take for granted. The metal bleachers, the roar of the crowd, the (gross) smell of hot dogs, the infield dirt blowing in my eyes…every bit of it is special to me on a whole ‘nother level.
Last night also marked the first time a newspaper reporter has covered the game, and seeing my boy’s name in print in association with his rock-star team’s blowout and his personal success is something I’ll be savoring for a while. Before cancer came into my life, I would have enjoyed reading the article, and likely would have forwarded it to our nearest & dearest, but this time, I’m carrying the feeling of that article along with me, inside my heart, in that little space where the gratitude lies.
I was flipping through my old Caring Bridge blog, and happened upon this entry, which seems even more prescient a year later. I wrote this on the morning of my mastectomy, before leaving for the hospital. No doubt I was antsy, preoccupied, and ready to get the show on the road that morning. It seems appropriate to reprint it today, in light of the theme of today’s blog.
I realize that when cancer comes into one’s life it disrupts everything and changes “the normal” forever. Dr Dempsey, my superstar breast surgeon, told me you no longer schedule cancer around your life, you schedule your life around your cancer. Life takes a backseat to war.
With cancer, I join a club that I never signed up for and for which I never wanted to become a member.
No matter, I now have a new normal. The new normal is all about taking care of what’s most important. We hear this all the time, but when you really put it into play in your own life, you know exactly what it means. For me, it means facing this beast head on and telling the bastard repeatedly that it doesn’t stand a chance. It means never once, not even once, considering that this cancer will win. It’s not even in the game.
It also means all the pithy stuff you hear about, like savor every day, make the most our of whatever you’ve got. That’s also true. For me it means truly embracing and enjoying my kids and my family, and letting my friends into my life — warts & all — on a whole new level. Y’all may well see my house a mess, which doesn’t happen much. You may see me in a grumpy mood (ok, you’ve seen that, esp on the tennis court!). You may see me just a teensy bit vulnerable, but only for a short time so don’t expect a repeat performance. No matter what, there is a new normal, and I’m all over it.
As if the tornado wasn’t bad enough…
Posted: June 14, 2011 Filed under: breast cancer, infection | Tags: AL East, Alex Rogriguez, Antibiotics, Dustin Pedroia, Freeman Hospital, fungus, hurricane categories, infection, infectious disease, Jacoby Ellsbury, Joplin tornado, mucormycosis, mycobacterium, psychological effects of cancer, PTSD, recovery, Red Sox Nation, survivor, tornado EF-5 1 CommentI feel a weird dichotomy of emotion when a friend hears about a rare and hard-to-treat infection and thinks of me. On one hand, it’s nice that my friends are the sort of people who know what’s going on in my life (I guess being a blabbermouth and having a blog help). On the other hand, it’s a weird feeling to be the one associated with the rare and hard-to-treat infection.
No matter, the horse is out of the barn, and the fact of the matter is that I did indeed have a rare and hard-to-treat infection, I am a blabbermouth, I do have a blog, and my friends rock.
So when the news broke that several people in the wake of last month’s giant killer tornado in Joplin, Missouri, have contracted a rare and hard-to-treat infection, my name came to mind. Perhaps this provides a bit of perspective for me. On many levels. It reminds me that while I’ve been through a lot, I also have a lot for which to be grateful. Namely things like this: #1, I wasn’t involved in the devastation of that giant killer tornado. #2, my rare infection was hard to diagnose but not especially hard to treat; just a giant pain in the ass. #3, my rare infection wasn’t deadly, as the one in Joplin is. #4, my rare infection is gone, baby gone. And, because I like odd numbers in lists, #5, I’m done with the 267-day course of oral antibiotics needed to treat my rare, pain-in-the-ass infection. Oh, if only I got paid extra for using hyphens in my modifiers.
The giant tornado last month in Joplin stirred up a lot of soil in its destructive path, and it uncovered mucormycosis, a deadly fungus among us. Like most bacteria and fungus, mucormycosis is all around us but only affects people who are already limping along with weakened immunity. The proverbial kicking a man who’s already down. It seems to prey upon people with diabetes, leukemia, lymphoma, and AIDS as well as those who have had an organ transplant and those who engage in chronic steroid use (Alex Rodriguez, you better be careful).
I must digress here for a moment about the mighty A-Rod. We don’t like him much in our house (understatement of the year, right there). Not just because we are die-hard, hard-core Red Sox fans and he’s on that other AL East team. You know, the one that wears those gawd-awful pinstripes. Ick. Well, A-Rod, in our opinion, typifies everything that’s wrong with pro sports: the drugs, the attitude, the disdain for the very fans who provide him job security. Imagine our surprise and delight when we found this yesterday:
An A-Rod baseball card, chewed to bits by our little dog Pedey. I love it! It’s even funnier because that little dog is named for Payton’s favorite Red Sox player, Dustin Pedroia. The idea of Pedey going after A-Rod fills my heart with pride. I’ve said before that Pedey is not much like his namesake: he’s lazy and clumsy with a ball, but in this case, Pedroia would be proud of this little dog for pouncing on A-Rod and tearing him to bits!
As long as we’re digressing for baseball-related ramblings, I might as well post a pic of my boy-crush, Jacoby Ellsbury. It’s been a while, and I know my loyal readers have missed him. Here ya go.
You’re welcome.
Ok, back to the Joplin tornado and its unwelcome sidekick. The tornado was a big one. An EF-5 to be precise. The EF scale refers to the Enhanced Fujita scale, which was developed at the Wind Science and Engineering Research Center at Texas Tech University. Yay Red Raiders. I don’t know much about the tornado scale, being a bit more familiar in this neck of the woods with the Saffir-Simpson Hurricane scale, but a quick peek on Wikipedia tells me that an EF-5 tornado means the storm has winds in excess of 200 mph. A bad-ass, scary storm, to be precise.
The May 22nd tornado cut the city of Joplin roughly in half with an estimated 7-mile-long by 1-mile-wide swath. It moved slowly and stayed on the ground rather than touching down and moving back up. All of these factors combined equal untold destruction, a death toll of 151 people, and the unleashing of a nasty fungus.
Eight tornado victims have contracted the mucormycosis, although public health officials won’t make an official link between the fungus and the tornado. Four of the people who tested positive for mucormycosis have died. It’s a nasty bug that spreads fast and can invade the blood supply of its victims, who typically have injuries and secondary wound infections. Sound familiar? Ugh. The rush of feelings and memories this topic evokes roars in my head much like a tornado. I think my PTSD is showing.
The mycormycosis fungus is usually found in soil and wood and enters the body either through a puncture wound or when a person breathes in mold spores. The dirt or vegetation becomes embedded under the skin, and mold is actually found in the wounds of people who have this bug. In some cases, wounds that had been stitched up after the tornado had to be reopened to clean out the contamination. Again, sound familiar? The incubation period is a little shorter on the fungus compared to the mycobacterium, and hopefully the fungus presents itself faster than the myco; both times I’ve been tested for that damn myco it took 6 weeks to present itself.
People with weakened immune systems who come into contact with this fungus have a mortality rate as high as 90 percent. Yes, you read that right: 90 percent.
It’s strange how the spores of this fungus look almost artistic under the microscope, yet can wreak unimaginable havoc on the human body. Compare that to my bacteria’s photo and you can see how vastly different these bugs appear under the microscope and why I have enormous respect for my sweet infectious disease doc. You rock, Dr Grimes! 
Because the mucormycosis fungus is so rare, medical research is limited, and treatment is simple but fraught with complications. Treating it sounds eerily familiar to me: confirm the bug, excise the affected tissue via surgery, and administer long-term and powerful antibiotics. Same plan I followed for the mycobacterium.
The Centers for Disease Control and Prevention said Friday that it is conducting tests to help investigate the infections, which are so uncommon that even the nation’s largest hospitals might see only one or two cases a year. In fact, Dr Ewe Schmidt, infectious disease specialist at Joplin’s Freeman Hospital, said that in 30 years of practice, he’s seen 2 cases of mucormycosis, both of which occurred in patients who had untreated diabetes.
“To my knowledge, a cluster like this [several cases of the fungus] has not been reported before,” said Dr. Benjamin Park, head of the CDC team that investigates fungal diseases. “This is a very rare fungus. And for people who do get the disease, it can be extremely severe.”
I’m so glad my rare infection wasn’t this deadly fungus. I’m even more glad that my rare infection is gone. And I’m so glad this guy and his dog survived the storm and the deadly fungus.
One year ago today
Posted: May 13, 2011 Filed under: breast cancer, drugs, food, infection, kids, pets, Surgery, tennis | Tags: Bactrim, blog, breast cancer, cancer battle, cancer diagnosis, champagne, coconut cream pie, DIEP, dogs, family, hospital, Houston, infection, infectious disease, IV antibiotics, kids, kids dealing with mom's cancer, lymphedema, mastectomy, Methodist Hospital, microsurgery, minocycline, Moet, mycobacterium, nausea, new boobs, plastic surgeon, plastic surgery, post-mastectomy, reconstruction, recovery, stress, surgery, survivor, tennis 12 CommentsY’all know I’m a milestone-observing kind of girl. I’ve written about my cancer-versary, about a revelation, about week-old recollections after The Big Dig, aka my reconstruction, and returning to the tennis court after a long absence full of longing.
I’ve written about the anniversary of my sweet mama leaving this earth. That was early on in my blogging, and I hadn’t mastered the art of inserting photos. The photos of her are woefully displayed, and in my free time (!) I need to go back and fix them. She deserves better.
I’ve also observed the end of the worst year of my life. “Don’t let the door hit ya” was my message to 2010 as it went out like a lion. A mean, underfed, on-the-hunt-for-victims lion. Almost halfway through 2011 and I’m happy to say it’s turning out to be a much better year. Course, we didn’t have far to go to make it better than its predecessor.
Back to the current milestone. One year ago today, I said bye-bye to my breasts and was the lucky recipient of a flat–but cancer-free–chest. This was me, this time last year. On this very day (although it wasn’t a Friday, it was May 13th. Having a bilateral mastectomy on Friday the 13th would be cruel).
Trevor snapped this photo of me waiting for my surgery, in the holding pen before moving to a pre-op room. My brain was swirling with lots of thoughts, too many thoughts, and I was likely firing off a quick email to our BFF Ed with some last-minute kid-wrangling instructions. Notice the pink notebook in my bag: my cancer book, full of pathology reports, doctors’ notes, research, and bills. Bills, bills, and more bills. I think the current estimate of the cost of my last year medically is in the range of $260,000. And we’re not done spending yet.
One year ago today, I wish we’d thought to take a close-up shot of my chest instead of the deep wrinkle snaking across my forehead. My chest would never be the same, and would become a major battleground–and that was after the mastectomy. If I’d seen that pic before going under, I would have asked Dr Dempsey, breast surgeon extraordinnaire, to give me some Botox while she was in there. Yikes.
I didn’t know what to expect from the surgery, other than the basics. With subsequent surgeries, I’ve learned that actual procedures are available for viewing on youtube and I’ve watched a few. Gross. But amazing.
All I knew, really, was that I had breast cancer and I wanted it gone. I could have had a lumpectomy, but chose the slash-and-burn option instead. I’m not a half-measure kind of girl, and the idea of just taking a part of the infected breast instead of the whole thing wasn’t anything I ever seriously entertained. Slash-and-burn meant taking both breasts, even though the cancer was only detected in the right one. Only. Ha! Good thing I lost the pair, because the post-mastectomy pathology showed the left one had some problems, too. If you can call an area 5 cm in diameter full of cancerous junk a problem. I can, and I did. Little did I know then, one year ago today, that pretty much anything that could go wrong with my post-surgery self would go wrong. As my nurse practitioner friend Laura says, “Your case certainly has not been textbook.” Truer words were never spoken, but we didn’t know that one year ago today.
Because there were only 3 weeks between my diagnosis and the mastectomy, and because most of that time was consumed with tests, tests, and more tests, there wasn’t a lot of time for freaking out or being scared or crying about my fate. Not that I would have done any of those things anyway. There was a problem, and we were going to fix it. ‘Nuff said. I had a great team–breast surgeon, plastic surgeon, and oncologist– and was in a nationally ranked and highly acclaimed hospital. Course, I’d end up adding a kick-ass infectious disease team, home-health care nurse, a beloved lymphedema specialist, and wound specialists to my team before it was all said & done.
The week before surgery, Payton turned 11
and Macy & I pampered ourselves with a Chinese foot massage.
I squeezed in as much time as I could with my girls


 I didn’t know it would be a while before I did anything like this with my favorite girl.
I didn’t know it would be a while before I did anything like this with my favorite girl.
Going into surgery one year ago today, I had no idea that I’d end up spending nearly a month more in the hospital and undergo 3 more surgeries; minor surgeries compared with the mastectomy, and of course reconstruction was way off in the distance, with even more days in the hospital. I had no idea how much I’d miss my kids while hospitalized
 and my dogs (and their friends).
and my dogs (and their friends).
I had no idea how many times I’d need the special parking place.
I had no idea how much infinite kindness my friends would bestow upon me. We were on the receiving end of many, many meals delivered to our house, a kindness for which I’m so grateful. The rides to & from my kids’ activities helped more than I could ever guess. The sleepovers and outings that my mommy friends provided kept my kids’ life normal when everything else around them was off-the-charts abnormal.
My cousin Teri’s hubby Tom made me more than one coconut cream pie. I ate a lot of this
Keith’s crab towers were chock-full of healing properties.
Yes, lots of champagne eased the way from being an average, suburban at-home mom to becoming a statistic. From regular woman to cancer vixen. From got-it-together overachiever to at the beast’s mercy. And my bubbly companion continues to ease the way, from cancer victim to cancer survivor. Cheers to that.
A week after surgery, I began to feel a bit more human and was blown away by my little girl wearing a pink ribbon on her shirt–all her idea, BTW–to school every day. 
I was not enjoying the amount of time spent doing this:
although Pedey enjoyed every lazy minute of my recouperating.
Seeing me in jammies all the time gave Macy an idea: she could raid my jammie drawer and wear them herself. 
I’m not sure I ever got that pair back from her.
I certainly have learned a lot over the last year. Things I never knew I would have to learn, like the difference between invasive ductal carcinoma and in situ carcinomas. Like how a tumor is graded to determine the stage of the cancer. Like cure rate statistics and recurrence stats. Like how fine a line there is between the science of medicine and the art of medicine. Like how fighting a wily infection could be even worse than fighting cancer.
The crash course in all things infection-related was a big education. A very big, most unwanted education. My biggest lesson in this arena is how many unknowns exist. I wanted to know when, where, how, and why I got this infection. No one knows for sure. I wanted to know why it took so long to diagnose it, and why so many drugs have to be involved. I learned that my oncologist could have me all my drugs delivered to my doorstep via UPS. I learned to love vanocmycin and to depend on probiotics. I learned to eat breakfast as soon as I got up, hungry or not, because I needed to time the antibiotics right so they hit an empty stomach. I learned that morning sickness-style nausea doesn’t go away as the morning changes to afternoon and then to evening. I learned that there was nothing, not one single thing, I could put in my stomach to ease that awful nausea. I learned that washing those drugs down with alcohol doesn’t make me feel worse; that in fact it made me feel a whole lot better. I learned to develop a schedule and a rhythm to taking my antibiotics every 12 hours for 267 days. 
I learned that “We’re discontinuing the antibiotics” are the sweetest words I’ve heard in a long time. I’ve learned about the complete and utter relief of dumping my remaining oral abx out, because I don’t need them anymore.
That’s the tip of the iceburg, or what my friend Michele would call “a booger’s worth” of the practical things I’ve learned. The topical aspects of changing one’s status from normal person to cancer patient. Then there’s the other side of it.
There’s the stuff I’ve learned in the last year about the unquantifiable side of a serious illness. The depth of inner strength required to get through something like this. The well of emotion that accompanies the clinical stuff. The patience and fortitude I didn’t know I had (although I’m still working on the patience part). The measure of gratitude toward the people who’ve helped along the way. The unbridled joy of making new friends in the midst of a shitty situation. The passion for writing, long dormant in the day-to-day of child-rearing, and the love of blogging. The understanding that my doctors are just regular people under those scrubs & white coats, and while they’re full of knowledge, there’s a whole ‘nother side of unknown things for which they make an educated guess and hope for the best. And, I have to admit, how much fun I’ve had getting to know these people in the white coats.
While being diagnosed with breast cancer at age 40 certainly does suck, I’m lucky that I made the decision one year ago to not let that diagnosis define me or impede me living my life. There certainly were times in which I was miserable from surgery and infection, and down in the dumps about my limited capabilities during recovery. There were also times over the last year in which I thought for a second I can’t take any more–not one drop more of bad luck, rotten news, and beastly complications. But those times didn’t last long and they did not prevail. Cancer did not prevail. Not over me. No way. Nuh uh. That’s perhaps the most important thing I learned over the last year.
The best news in a long time
Posted: May 6, 2011 Filed under: breast cancer, drugs, infection, tennis | Tags: Antibiotics, infectious disease, mycobacterium, nosocomial infection, Pommery, post-mastectomy infection, Seinfeld, tennis, witch is dead, Wizard of Oz 16 CommentsAfter 267 days, I finally heard the words I’ve been dreaming about: “We are discontinuing the antibiotics.”
Cue the hallelujah chorus.
I saw Dr Samo instead of Dr Grimes today, and he delivered the most-excellent news. He is my new best friend. All of the cultures run during The Big Dig came back negative, which means we can safely assume the post-mastectomy infection is gone. Yes, at long last, the mycobacterium has been vanquished.
Let me say that again: the infection is gone. I’m cured.
No more twice-daily dose of minocycline and bactrim. No more nausea. No more planning my consumption of food & drink around my doses. No more remembering to take my drugs. No more antibiotics.
Oh, happy day!
I’m still in a mild state of shock, or maybe just slightly buzzed. Could be the celebratory champagne straight away after returning from the medical center (duh), and the margarita at my tennis team’s end-of-season lunch. 
We broke out the good stuff and gathered our close circle of friends who would never say “it’s too early” and question the wisdom of popping a cork at 11 a.m. To Amy, my chief medical correspondent and chauffeur to & from appointments: thank you. For everything. To Jill & Keith: thank you for rushing right over, then leaving as soon as the bubbly was gone. But for planning to come back with dinner.
My tennis team’s luncheon was already planned, but how fun to celebrate my big news with some of my favorite girls? And how cool that they gave me a huge, signed tennis ball? Thanks, girls!
The infection is gone. Ding dong, the witch is dead.
I half expected the citizens of Munchkin Land to come out and dance their little legs off and sing in their froggy voices to celebrate.
I admit, I’ve been wondering all week if my visit to the infectious disease doc today would result in the end of the abx. I was trying to not get my hopes up, and while I knew not to expect it, I would have been disappointed if they’d said keep on swallowing those pills. No matter. It’s all good now.
I will also admit that when the nurse was taking my BP and temp and asking me the reason for my visit, I felt funny saying “yes” to her question of “are you here to see if it’s time to get off of the antibiotics?” It was almost too much to hope for. Almost.
Then when Dr Samo uttered those glorious words of “We are discontinuing the antibiotics,” I was stunned. It was a bit surreal. Once I grasped what he’d said, my first thought was that “discontinuing” meant taking a break, not stopping them altogether. 
It was almost too much to take in.
As my best buddy Ed said, “I feel I should shove you and yell ‘Get Out!’ like Elaine on Seinfeld.
“Get Out!” indeed.
The end of the antibiotics is like an end of an era. My life has revolved around them for so long now–one week shy of a year, in which I’ve been on some form of abx, whether oral or IV. Nearly a year on some pretty powerful drugs, and none of them the fun kind. Nope, these are the ones that tear up your stomach and make your insides cry like a baby.
But no more.
Big sigh.
The fat lady can sign her heart out right now.



















