9/11 and cancer
Posted: August 26, 2015 Filed under: Uncategorized | Tags: 9/11 first responders, cancer and 9/11, Ground Zero, Marcy Borders, Michael McAuliff, September 11, Stan Honda, toxic dust, World Trade Center 4 CommentsRemember seeing this photo in the aftermath of the terrorist attacks on the World Trade Center on September 11, 2001?
Marcy Borders, who came to be known as “the Dust Lady” survived the WTC attack after fleeing her office on the 81st floor of the North Tower. She was 28 years old. That terrible day set off a chain of events that ended tragically: on Monday, Marcy Borders died, at age 42, from stomach cancer.
Borders suspected a connection between the terrorist attacks and her cancer. In an online interview, she wondered if her experience on that terrible day caused her cancer: “I’m saying to myself, ‘Did this thing ignite cancer cells in me? I definitely believe it because I haven’t had any illnesses. I don’t have high blood pressure … high cholesterol, diabetes. … How do you go from being healthy to waking up the next day with cancer?”
That’s a question many of us have asked. Whether young or old, the question of how one goes from healthy to cancer-ridden remains, and that question can haunt those of us who have stared into the eyes of the beast that is cancer.
For those who were at Ground Zero, that haunting question becomes a common refrain. It’s hard to know just how many cancer diagnoses resulted from events surrounding the terrorist attacks, but we do know that first responders and civilians fleeing the towers were exposed to a nasty combination of carcinogens. This toxic dust is likely responsible for the fact that people present in the terrorist attacks have gotten certain cancers — skin and prostate cancers as well as non-Hodgkin’s lymphoma and mesothelioma — at significantly higher rates than people in the regular population. Even now, more than a decade later, the lingering health effects remain unknown, but experts suspect the full extent of cancer and 9/11 will begin to emerge, as it has with Marcy Borders.
Photographer Michael McAuliff was also at Ground Zero on September 11, covering the events for ABC News. He too wondered how his health was affected by the dust that covered Marcy Borders and everyone else in the vicinity. He collected and saved the dust that covered him as he worked on September 11, 2001, and recently submitted the dust and his computer bag he carried that day for testing. When the test results arrived, McAuliff discovered:
“About half the material was ‘non-fibrous’ including polystyrene foam, vermiculite mineral, combustion product (carbon soot), mineral dust of gypsum, calcite, dolomite and quartz. The other half was fibrous material including “cellulose (wood and paper fragments), fibrous glass such as glass wool with yellow resin coating, Fiberglass, colorless mineral wool, refractory ceramic fibers, limestone, calcites, carbon fibers, synthetics (including fragments of cloth) and chrysotile asbestos associated with the lime and carbonate insulation debris. Also found were ‘additional chemical signatures of silicates, kaolin clays, pigments (TiO2), calcites, dolomites, carbonates, metal complexes (sub-micron chromium, aluminum/iron matrices) and chrysotile asbestos.’ Metals included small amounts of lead, chromium, zinc and cadmium.”
McAuliff seems to have dodged a bullet and has received a clean bill of health. Unlike Marcy Borders.
Surviving the terrorist attack was just the beginning of a long battle for her. In an interview, Borders said “it was like my soul was knocked down with those towers.” Her battered soul endured depression and drug addiction. “My life spiraled out of control. I didn’t do a day’s work in nearly 10 years, and by 2011 I was a complete mess. Every time I saw an aircraft, I panicked. I started smoking crack cocaine, because I didn’t want to live.”
Ten years later, Borders decided she did indeed want to live, and in April 2011 she entered rehab. She worked hard to reclaim her life and move forward. She got sober and committed herself to putting that terror behind her, saying “The anniversary of (9/11) gives me no fear. I’ve got peace now. I’m not afraid of anything. I try to take myself from being a victim to being a survivor now. I don’t want to be a victim anymore.”
Rest in peace, Marcy Borders, and know that you are much more than “the Dust Lady.” You are proof that we can endure terrible things and come away with peace.
15 things
Posted: July 11, 2015 Filed under: Uncategorized 12 CommentsI’ve been in need of a reason to sit down at my computer and bang out a blog post, but I’ve been lazy. Chalk it up to summertime and its glorious release from the grind of our daily schedule. Thankfully, the blog challenge put forth by Nancy’s Point and taken up by Marie motivated me to shake off that laziness and get to it.
Drumroll, please.
15 things. Random things about me. I know y’all have been itching to know more about the inner workings of my particular brand of crazy. Have at it.
1. I love animals and have been accused of loving critters more than people. To which I say, it depends on the person.
2. Meat in any form grosses me out, big time (correlation to fact #1?). I still cook chicken and turkey for my family but wear latex gloves to handle the raw stuff, and the process of picking out a package of meat at the grocery store usually makes me want to barf. Because we have a pet pig, pork is obviously a no-go in my house.
3. Being organized makes me happy; chaos makes me hyperventilate a little.
4. I have an addiction to lip balm. I have tubes of my favorite kind stashed everywhere: in the kitchen, in my car, on the patio….I leave the lids off so I can grab the tube, swipe it on, and keep moving.Every chance I get, I visit a different grocery or drug store to look for my favorite kind. When it seemed to be getting scarce, I ordered an embarrassing quantity online. When my favorite girl saw that stash she asked if I had robbed a Blistex salesman. Ha, ha, very funny.
5. I love books and am torn between relishing the heft of a real book and being seduced by the convenience of ebooks.
6. Patience is not one of my virtues. Being stuck in line drives me crazy, as does a pokey driver in the left lane or a string of people walking slowly.
7. Similarly, I struggle with diplomacy. I want to say the right thing, the kind thing, but the harsher, more direct version is what comes to mind first.
8. I would love to speak a second language. I took Spanish in high school, but my teacher was a childhood friend of my dad’s and I had yet to master the art of working hard despite the easy out. Or easy A, as the case may be.
9. Physical activity lights my fire. I love a grueling workout, a multi-hour tennis match, an afternoon digging in my yard.
10. I get a huge dose of satisfaction from being productive and am not so good at sitting still.
11. I’m a foodie and am usually thinking about lunch as I’m eating breakfast. I used to tease my sweet mama for doing that, and now I do it, too.
12. I didn’t like beer for more than 20 years, but being on long-term antibiotics after a nosocomial infection changed my taste buds. There are few things better than the first sip of an ice-cold beer.
13. While on the topic of booze, I should confess my undying love for champagne. It makes every occasion a special one.
14. I’m a germophobe. People coughing or sneezing in public makes me cringe, as does the idea of sharing a cup with someone else. People who share a toothbrush are like aliens to me. I cannot wrap my head around that concept. Eww.
15. I love lists and always have a to-do list going. Perhaps that’s why the idea of a post listing 15 things appealed to me.
Rain, rain go away!
Posted: May 28, 2015 Filed under: new house | Tags: #houstonflood, Bellaire, Brays Bayou, Hurricane Ike, Meyerland, state climatologist, Texas flooding 14 CommentsThe rain has been relentless in my part of the world. H-town has made national news this week, with photos of our soggy city and Mother Nature’s destruction relaying the misery.
Here’s a shot comparing the same freeway before and after our epic rainfall.
And another before-and-after shot in the Meyerland area (although the way the photographer arranged the photos, it’s an after-and-before shot).
This photo was taken Tuesday morning near the Museum District. MacGregor is the street we exit to go to the Houston Zoo. It’s crazy weird seeing such familiar sites under so much water. The state climatologist (yes, that is a real job) estimates that Texas has received more than 7.5 inches of rain in May.
We haven’t seen rain like this since Hurricane Ike, which hit my city in 2008. In fact, the Houston Weather Service has not issued a flash flood emergency since Ike. Until this week. We have had rain in biblical proportions. Some areas of Houston were drenched with 11 inches of rain Monday night and Tuesday morning. One of our local weather nerds equated that rainfall to 162 billions of gallons of water.
In the suburb I call home, the aftermath of the storm was less dramatic. Thankfully. Our house backs up to a bayou that has a small stream running through it; normally we can’t see the water out our back windows. This is what it looks like on a normal day (sometimes you can even catch a glimpse of sweet Pedey, sunbathing or napping).
And this is what the view over my back fence looked like on Tuesday. 
See that small gravel patch in the middle of the photo below? That’s the end of the little gravel road we use to cross the bayou. The rest of that little road is completely under water. 
It was hard to tell just how deep the water was, and I had a fleeting thought about crossing that little road to get a photo of the other side of the bayou. A very fleeting thought. Several steps in, the water was halfway up my boots.
Several steps in, the water was halfway up my boots.
A few more steps, and the water was coming in my boots.
My beloved bayou was flooded. I wondered what this meant for the wildlife we love to observe just beyond our back gate. No sooner did I wonder when I heard a splash and saw a young deer swimming across the bayou. I watched to make sure she got across safely and made a mental note to throw some kale and dried corn over the fence for her. The lush foliage and wild berries she normally nibbles on were washed out.
A parting shot of my bayou after the big storm is quite serene and lovely, despite the epic rain.
Angelina’s Diary of a Surgery
Posted: March 24, 2015 Filed under: breast cancer | Tags: Angelina Jolie, Angelina Jolie PItt, BRCA, BRCA1, celebrities with cancer, losing a parent to cancer, prophylactic mastectomy 12 CommentsI just read Angelina Jolie Pitt’s op-ed in The New York Times about her second preventative surgery: to remove her fallopian tubes and ovaries. Just as she did with her prophylactic bilateral mastectomy two years ago, Jolie Pitt writes articulately and openly about her laparoscopic bilateral salpingo-oophorectomy, using imagery and opinions that those of us who have walked in her shoes immediately understand.
She writes, “The beautiful thing about such moments in life is that there is so much clarity. You know what you live for and what matters. It is polarizing, and it is peaceful.”
So much clarity. Amidst untold chaos and unimaginable confusion, there is clarity.
She recounts her consultation with the GYN surgeon, who had also treated her mother: “I last saw her [the surgeon] the day my mother passed away, and she teared up when she saw me: ‘You look just like her.’ I broke down. But we smiled at each other and agreed we were there to deal with any problem, so ‘let’s get on with it.’”
I had a similar encounter with someone who cared for my own sweet mama during her cancer treatment. The woman who was my mom’s radiation tech is now a nurse in my orthopedist’s office. I knew as soon as I saw her face that she was the kind practitioner who blasted pointed radiation into my mom’s beleaguered body five days a week for weeks on end. When I encountered her in the orthopedist’s office, I was thrown for a moment because she was out of context. But before long we realized who each other was, and she said the same thing to me that Jolie Pitt’s mom’s surgeon said to her: “You look just like her.”
Stupid fucking cancer.
When Jolie Pitt wrote about her mastectomy in May 2013 she cast the spotlight on the issue of femininity being defined by body parts. After her mastectomy she wrote: “I do not feel any less of a woman. I feel empowered that I made a strong choice that in no way diminishes my femininity.” With her latest surgery, Jolie Pitt casts the spotlight on another jarring and difficult result: forced menopause.
Becoming menopausal decades before its natural occurrence is unpleasant, to say the least. The physical and emotional ramifications of forced menopause suck. Really suck. There is no easing into the myriad effects, which can include hot flashes, night sweats, increased sweating, sleep disturbances, mood swings, urinary tract infections, sexual disfunction, memory loss, difficulty concentrating, back pain, joint stiffness, and fatigue. As if that’s not enough, throw in the accelerated aging: loss of elasticity in skin, lack of collagen, hair loss, brittle nails, diminished muscle tone, slower metabolism, and weight gain. Suck. At a time when many women are claiming the best version of themselves (“40 is the new 20!” “I’ve finally come into my own!” et al), early menopause creates instant grannies. Suck. If anyone can shed light on the ugly truths of forced menopause, my money is on Angelina. Yes, she has unlimited financial means and resources unavailable to the average cancerchick, but she also has a platform for educating the masses and she’s gonna use it. Hooray!
At the time of this publishing, there were 321 comments on her story; by the end of the day that number will have climbed. The handful of comments that I scanned were positive, but there are some who chastise her for her choices. I’m always amazed at how ugly people can be with the anonymity that our online world provides. How nice it would be if those cowardly, overly opinionated haters could really digest Jolie Pitt’s reasoning and respect her choice. How nice it would be if they would re-read the last sentence in this segment of her latest essay:
“I did not do this solely because I carry the BRCA1 gene mutation, and I want other women to hear this. A positive BRCA test does not mean a leap to surgery. I have spoken to many doctors, surgeons and naturopaths. There are other options. There is more than one way to deal with any health issue. The most important thing is to learn about the options and choose what is right for you personally.”
Choose what is right for you personally.
What works for you may not be the same thing that works for me, or for your neighbor or your cousin or the woman who works at your favorite Hallmark store. Cancer, like any disease, is an immensely personal issue, and any and all decisions resulting from a diagnosis should be personal.
A solution on paper only
Posted: March 5, 2015 Filed under: drugs | Tags: chronic pain, hydrocodone, pain management 10 CommentsThis is a real-life tale of the fall-out from the FDA restricting the use of hydrocodone, better known by the brand names Vicodin, Lortab and Norco. Notices like this hang from cabinets in every doctor’s office I have visited. 
I am not a junkie. I am not an abuser of painkillers. prescription or otherwise. I have no desire to self-medicate with painkillers. That’s what wine is for. Duh.
Millions of people do self-medicate with Vicodin, though, and last Fall the U.S. government stepped in to try to dethrone Vicodin from its perch as most prescribed medication in the entire country. Vicodin is the Miss America of painkillers. In 2010, doctors in the United States wrote 131 million prescriptions for Vicodin. First runner-up in the Miss America of Prescription drugs was Zocor, a statin that trailed Vicodin by 36 million sripts.
So, too many people asked for Vicodin, too many doctors complied, and an epidemic of misuse occurred in which drug-overdose deaths claimed more lives than car crashes. In drug-overdose deaths, an estimated three-fourths involve painkillers, according to federal statistics. So the government stepped in and reclassified hydrocodone as a Schedule II drug, alongside the most powerful drugs, like morphine and oxycodone. With that reclassification, it became damn near impossible to get a prescription for Vicodin. No longer could a doctor call in a prescription for Vicodin. No longer can a physician’s assistant prescribe Vicodin. No longer can Vicodin just sit on the shelf next to all the other drugs; now it must be locked up in a vault.
The sticky wicket with drugs like hydrocodone is that it is one of the most effective drugs against pain, but it is also has the potential to be the most addictive of the prescription drugs. No doubt the misuse of painkillers like Vicodin is a problem and can ruin lives. However, pain has that same potential. Whether chronic or situational after a surgery, pain can ruin your life.
I know, because I live it.
I have chronic pain, from a misaligned and thrice-operated-upon knee as well as from carpal tunnel syndrome. Every single day I have pain. Not just a little bit, either. And not the kind that is alleviated by OTC meds or Tylenol 3. But the kind that not only affects my everyday life but has also changed who I am. Studies show distinct links between pain and anxiety, and that chronic pain destroys our physiological ability to experience joy. This I know to be true. I am at war with my body, and I am losing.
When the pain from my carpal tunnel became so bad that I could hardly use my hands and fingers, especially first thing in the morning, and when the pain awakened me more than one time every night, I knew I had to schedule surgery. I’ve been putting off the CTS surgery for a while because, quite frankly, I am so done with surgeries. I am so over surgeries. I can’t even. Yet I must.
I got several recommendations for hand surgeons and chose Dr P, who did CTS surgery on one of my fellow gym-rat friends. She was back in the gym, albeit at a reduced pace, less than a week after surgery. That reassured me and got me into the exam room for my consultation with Dr P.
Along with my consult, I got a nasty surprise: not only do I have carpal tunnel syndrome, I also have cubital tunnel syndrome, and it too requires surgery.
Yeah, I’m an overachiever that way.
I’d never even heard of this ghastly cubital tunnel syndrome before, and am guessing you haven’t either (it is the second-most common nerve entrapment in the entire human body, but is very often misdiagnosed). It’s basically nerve entrapment of the ulnar nerve, which runs from the side of the neck to the fingertips. The ulnar nerve passes through the cubital tunnel behind the inside of the elbow and runs all the way down the forearm and into the hand. This nerve provides feeling to the pinky and ring fingers as well as working the muscle that allows us to pull our thumb into the palm of our hand.
There are two ways to fix cubital tunnel syndrome, and they both suck. In medial epicondyltetomy, the bony bump of the inner elbow is removed to allow the ulnar nerve to slide through the cubital tunnel (translation: the surgeon shaves part of your elbow off in order to re-route the ulnar nerve). That seemed pretty horrifying to me, yet the other method is even worse. In ulnar nerve transposition, the surgeon creates a brand-new tunnel for the ulnar nerve by carving a trench in the flexor muscles of the forearm and relocating the ulnar nerve from the cubital tunnel into the newly carved tunnel.
In my case, Dr P won’t know which procedure he will need to do until he gets in there. His plan is to make a 6-inch incision along the inner part of my arm between my shoulder and elbow. Then he’ll have a little look-see and decide which form of torture best suits my jacked-up body.
So, just to recap: I’ll be having not one but two surgical procedures: one to correct the carpal tunnel syndrome, and the other to reroute my errant ulnar nerve. Both surgeries involve the usual cutting, splaying, digging in, and stitching up flesh (and perhaps bone, too). Both surgeries involve jacking with nerves (ouch). The cubital tunnel surgery involves cutting through muscle when the ulnar nerve transposition is called upon to solve the problem. Both methods of correcting the cubital tunnel issue involve physical therapy (in the case of ulnar nerve transposition, PT can last upwards of four months).
My experience with surgeries that involve nerves, bones, and muscle is that the result is pain. Lots of pain. Which brings us back to the government reclassifying hydrocodone.
In the course of discussing the two surgical procedures with Dr P, I asked about pain management. I was reeling from the cubital tunnel diagnosis and the nasty surgery it entails, as well as the hard recovery involved and was totally unprepared to hear him say that his standard of care for pain control — after cutting nerves and potentially shaving off bone and carving through muscles — is Tylenol 3.
Let me repeat: cutting nerves, shaving bone, carving through muscle. A 6-inch incision. Tylenol 3.
Oh, hell no.
I gave him a brief synopsis of all my previous surgeries, which have involved cutting nerves, shaving bone, and carving through muscle, and informed him that Tylenol 3 doesn’t do shit for that kind of pain. He countered with an offer of a nerve block during surgery, to provide short-term pain relief. I shook my head in disbelief at the idea of a nerve block making more sense than a prescription for a small number of pills to be used at my discretion. We had reached an impasse.
He suggested I consult a pain-management doctor to discuss a stronger form of pain-killer. Again, I shook my head at the idea that involving another doctor — and adding another layer of expense, to me and my insurance company — made more sense than writing a prescription for a handful of pills.
Guess what? I happen to have a pain-management doctor, because that’s how we roll when we have chronic pain. You might think that a pain-management doctor could help a patient manage pain. But when I called my pain-management doctor’s office to request a stronger form of post-surgery pain-killer, his receptionist’s response was, and I quote, “I can tell you that’s not going to happen.”
I suspect what she meant was that because I has not seen him recently I needed a referral in order to make an appointment. I have learned the hard way how to read between such lines. So I called Dr P’s assistant and reported back. She called the pain-management doc with a referral and was told that I could come see the pain-management doc on March 16 — which is 10 days after my surgery.
I’m still wondering how that would help me.
Going in for surgery is stressful, on many levels. Worrying about pain control afterward should not be a part of that mix.
Here’s the bottom line about the lock-down on hydrocodone: there is no longer any difference between a patient who seeks a prescription for a short-term course after surgery/injury and those looking for a fix to get high. The new policy is reductive and buys into the punishing adage of a few bad apples spoiling the bunch. For patients like me, who want the peace of mind that comes with knowing adequate pain relief is available, the lock-down creates shame.
Having to beg for effective, short-term pain relief after a legitimately painful surgery creates shame.
As if that’s not bad enough, many pharmacy groups, pain consultants, palliative care specialists, and oncology specialists believe that the lock-down on hydrocodone won’t work. These guys realize that the lock-down will likely lead to different, possibly more devastating, problems. Those who seek hydrocodone for recreational use or escapism are going to find it, regardless of the reclassification. But those who need it situationally are shit out of luck. And that’s really shameful.
Mary Claire King
Posted: February 12, 2015 Filed under: breast cancer | Tags: BRCA, BRCA1, genetic marker testing, Mary Claire King, Myriad Genetics, podcasts, the breast cancer gene, The Moth 8 CommentsTwo new habits in my life brought a crazy-good, goosebump-inducing moment into my life last night, which illustrates the lovely possibility of finding something awesome in an otherwise everyday moment.
My two new habits: walking Pedey in the pre-sunset hour while listening to podcasts. Credit for the first habit goes to Pedey himself, who in his previous life in our former house was the laziest creature on Earth but who has developed a new leash on life (heh heh) since residing in our new abode. Credit for the second habit goes to my medical sherpa and dear friend Amy, who turned me on to the wonderful world of podcasts.
So last night, I was walking Pedey
listening to a podcast, and taking in the beauty of the evening. While much of the country is covered in snow, here in the Great State of Texas, it was a balmy 70-something-degree evening. This is what it looked like when Pedey and I headed out for our walk,
and this is what it looked like when we were nearing home.
Along our walk I tried to ignore the ever-present pain in my bum knee and the increasing discomfort in my hands from this wretched carpal tunnel syndrome. Instead, I forced myself to be present and to notice things like the shapes of the clouds in the darkening sky and the colors on display.
I smiled to myself because I didn’t have to rush home to make dinner (I’d cooked a double batch of chicken noodle soup for a friend whose entire family was felled by the flu). Instead, Pedey and I could linger while taking in the view.
The podcast was from The Moth, which for the uninitiated, features real people telling real stories from their lives, live in front of an audience without notes. These are regular people telling personal stories; you can hear the nervousness and emotion in their voices. Each Moth podcast typically contains several stories with a common theme. The one I listened to last night had four stories: a doctor faced with her own father’s memory loss; a man recounting his attempts to plan his Bar Mitzvah as a teenager; an archeologist who had a very personal run-in with the effects of climate change; and a doctor whose life is upended as she is on the cusp of a breakthrough in cancer research.
I had listened to the first three stories earlier in the day, while making the soup, and so had the last story to savor as I wrapped up my day with the twilight walk with Pedey. The narrator of the last story, Mary Claire King, told a compelling story that began on April Fool’s Day in 1981 when her husband dropped the bomb that he was leaving her to run away with one of his graduate students. The Kings had a 5-year-old daughter at the time, and the very next day Mary Claire was awarded tenure at Berkeley. Reeling from the announcement from her husband and processing the tenure award, she arrived home to find that their home had been burglarized. Her father had recently died, and her mother had just been diagnosed with epilepsy. Add to that chaos that she was due to travel from California to Washington, D.C., to present a grant proposal to the NIH for her research. Yowza. That’s what’s known as a class-A cluster.
A snafu in Mary Claire’s childcare for that trip to D.C. nearly brought her pursuit of the NIH grant to a halt, but thanks to some over-and-beyond help from her mentor and intervention by a kind — and über famous — stranger at the airport, she was able to make the trip, present the proposal and win the grant. I was still agog at her recounting of the airport encounter when she finished her story by saying “that was the beginning of the the grant that has become the story of inherited breast cancer and the beginning of the project that led to BRCA1.”
Wow.
Mary Claire King is the person who discovered “the breast-cancer gene.” She pioneered the genetic research that has completely changed the way breast cancer is diagnosed and treated. She has changed the lives of countless women, including the one walking her dog on a beautiful February night in the Great State of Texas. Crazy. And crazier still is the fact that she very nearly did not get on that plane to present that grant that would lead to one of the biggest medical discoveries of this lifetime.
I’m soooooooo glad she did get on that plane.
I have personally benefitted from Mary Claire King’s work, and there she was, in my earbuds, telling an incredibly compelling story, the majority of which has little to do with her groundbreaking research and her far-reaching progress in our frustratingly slow war on cancer. I don’t carry the gene that predisposes me to breast and ovarian cancer. Being free of the genetic predisposition doesn’t really change anything about my cancer “journey.” Despite not having the genetic predisposition, I nonetheless have had a bilateral mastectomy and a complete hysterectomy. I find some peace in knowing that my cancer wasn’t caused by funky goings-on in the 17th chromosome, and that I’m not passing that funky gene on to my daughter (and son). I don’t know what caused my cancer, but I’m fortunate to have had the resources to take the BRCA1 test to find out whether my 17th chromosome had funky goings-on that would indicate causality. I like knowing, even if it didn’t change the outcome or my choices in treatment.
Decades before breast cancer entered my world, King was hard at work to figure out how it worked and how to stop it. I love her. From 1974 to 1990, King worked to find a connection between genes and breast cancer. When she began this quest, the prevailing scientific explanation for cancer was a virus; no one thought it could be genetic. But King thought otherwise. She used her previous theory from her Ph.D. , which showed that humans and chimpanzees are 99 percent identical genetically, to pursue a genetic component to cancer. She believed that examiningt the DNA of women whose relatives had breast cancer could lead to a genetic link, and in the pre-internet era, she gathered information by hand and by word-of-mouth. She overcame obstacles from lack of funding to primitive research tools to derision as a female scientist. She prevailed. She rocks.
Those of us unfortunate souls whose lives have collided with a diagnosis of breast cancer or ovarian cancer know about the BRCA component. While a low percentage of breast cancer is genetic, the discovery of the BRCA component affects all of us in the Pink Ribbon Club. My cancer was not inherited, but I’m certainly glad I had the opportunity to learn that. Furthermore, the possibility of future breakthroughs in cancer research are promising. The solution to the cancer epidemic lies in people like Mary Claire King, long may they prevail.
Listen to Mary Claire King’s story on The Moth. It’s a good one.
World Cancer Day & Stuart Scott
Posted: February 4, 2015 Filed under: Uncategorized | Tags: Every Day I Fight by Stuart Scott, Jimmy V, Jimmy V Award for Perseverance, mycobacterium fortuitum, nosocomial infection, post-mastectomy infection, Stuart Scott, World Cancer Day 2 CommentsToday is World Cancer Day, and rather than rehashing my own cancer “journey” I’m thinking about Stuart Scott.
A longtime ESPN anchor, Scott was a familiar presence in my house. His wordsmithing appealed to me, as did his irreverancy. In a world populated by former jocks and professional windbags, Scott contributed a cool combination of intellectual breadth and liveliness. Scott’s colleague Dan Patrick once said about Scott that “he didn’t just push the envelope, he bulldozed the envelope.” I’m a fan of bulldozers.
Scott was diagnosed with appendix cancer in 2007. Yes, you read that right: appendix cancer. Weird and rare, there are an estimated 1,000 cases of appendix cancer in the United States annually, compared to nearly 300,000 cases of breast cancer every year in this country. Perhaps this is another reason I relate to Stuart Scott: between his appendix cancer and my post-mastectomy mycobacterium infection, we both faced the question of “who in the world contracts that??”
Stuart Scott wrote a book about his cancer “journey,” which explains his gladiator approach to confronting his disease. The cancer community is divided on the “battle” aspect of the cancer fight — some people love the idea of a cancer warrior while others are uncomfortable with the war metaphors — but one thing I know for sure: the cancer experience is a fiercely personal one, and no one has the right to tell another how to do it or which analogies to use.
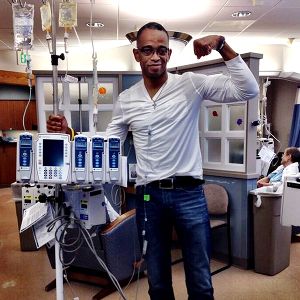
I read an excerpt of Scott’s book and am hungry for more. He was a gym rat, like me, and he leaned heavily upon his workouts during treatment, both for physical strength and for mental health:
“I can’t tell you how important it felt to go from the chemo infusion center to the gym. There were patients at the infusion center who were gaunt and too weak to walk. I wanted to hug them. I wanted to work out for them. It took about fifteen minutes to get to the gym from the infusion center, but I felt like I was traveling a great distance: from the land of the sick to the land of the recovering. I’d work out three or four times a week, but the most important workout was the one right after chemo. It was like I was proving a point: While you kick my butt, cancer, I’m gonna kick yours.”
In thinking about the name of one of the drugs in his chemo cocktail, Scott realized “The medical name of the medicine is fluorouracil, but they call it 5-FU. That’s what it said, right there: 5-FU. All right, I thought. A sign. FU, cancer.”
FU cancer. Indeed.
Scott continues: “My return to the gym felt kind of spiritual. I wasn’t really supposed to run since I was still connected to the port that was giving me my medicine. I looked down, and my eye caught the logo of the manufacturer of the machine I was on: LifeStyle. That word jumped out at me: Life. I thought back to the first thought I had when [diagnosed]: I’m going to die. But I was still here. And here I was, not forty-five minutes out of chemo, and I was in the gym, doing what I do. I started to run. What could be the harm? The disease wasn’t in control. I was.”
That sense of control is of epic importance in the cancer “journey.”
Scott explains it like this: “Mentally, I needed to be in that gym. I’d talk smack to cancer like Ali talked to his opponents. A third set of push-ups? Take that, cancer. Twenty full-out sprint pass patterns? Cancer, you ever run up against this? Some kicks and punches into the middle of the heavy bag after the elliptical? I got yer cancer right here! I needed to do that, not just to show my girls I was fighting for them, but also to show myself I had some control over the situation. ‘Cause cancer wants to take control from you. You’ve got to very purposefully stand your ground. That’s what going to the gym is to me. I decide, cancer.”
A few weeks ago I came across the late ESPN sportscaster’s speech about his cancer “journey” at the ESPY awards last summer. That speech is powerful. Here’s the link so you can check it out.
Scott was awarded the Jimmy V Award at last year’s ESPYs and joins an acclaimed list of courageous and inspirational people from various corners of the sports world. Perhaps his career as an on-camera personality gave him the extra flair that made him such an engaging speaker. Maybe that was just his personality. Either way, his speech is compelling.
The take-away message, for me, lie in these words from that speech:
“When you die, that does not mean that you lost to cancer. You beat cancer by how you live, why you live and in the manner in which you live.”
Stuart Scott taught me a huge and valuable lesson. He did die, but he did not lose. How he lived proves that. Today, on World Cancer Day, I honor Stuart Scott. While at the gym, I will think of his no-mercy approach. I will remember all the days in which I was that patient too weak to walk, and I will silently thank him for all the times he worked out in my stead. For all the times he went straight from chemo to the gym and said FU, cancer.
New year, new game
Posted: January 19, 2015 Filed under: cancer fatigue, Surgery, Uncategorized | Tags: carpal tunnel syndrome, CTS and hypothyroid, hypothyroidism, lateral release for dislocated kneecap, Maque knee surgery, osteotomy, Supartz, Synthetic synovial fluid, thyroid biopsy, thyroid nodules 13 CommentsTwo weeks into this new year, I am wrapping my head around a whole ‘nother challenge. This new game has nothing to do with cancer (for the moment, anyway — knock wood) but concerns the myriad ways my body challenges me. I refrain from classifying those challenges as failures, i.e., the many ways in which my body is failing me, because that is the new game: the mental side of physical illness.
I’m a fierce player in all aspects of the game that is confronting health issues. All aspects except the mental game. I suck at that part. Give me the worst-case scenario (mycobacterium fortuitum, I’m talking to you) and I will slay it. Give me a long, difficult road on which to travel, and I will keep on truckin’. But tell me that the only weapon I have in which to fight is my mind, and I’m hosed. Tell me to stay positive and look on the bright side, and I struggle. Offer me platitudes and I will want to punch someone. Outlook: not great.
Some of the news ways in which my body challenges (fails) me are minor: graduating to the bifocal club, or needing to hit the hay well before midnight. To those challenges I say let’s call a truce. But the bigger challenges are well, bigger. And more challenging. There are three bad guys vying for attention these days: the bad knee, the wonky thyroid, and carpal tunnel syndrome. Awesome.
The bad knee is acting up and acting out. Again. Three surgeries and countless rehab exercises mean nothing to that old hag. The misaligned kneecap is screaming for attention, and the missing cartilage is hunkering for its piece of the pie. Two very squeaky wheels in an already crowded field. The second round of synthetic synovial fluid injections did little to appease the missing cartilage.  Despite the giant needle being jabbed straight into the innocent flesh adjacent to the bone-on-bone area, relief evaded me. Upon reviewing my day-after-Christmas x-ray, my orthopedist shifted gears from a previous recommendation of partial knee replacement to osteotomy, which requires cutting the bone at the top of the tibia and using plates and screws to relocate it in its proper place. The one word that comes up when researching the recovery for this surgery: brutal. Standard care is crutches for two weeks and a cane for a month alongside endless physical therapy. Thanks but no thanks.
Despite the giant needle being jabbed straight into the innocent flesh adjacent to the bone-on-bone area, relief evaded me. Upon reviewing my day-after-Christmas x-ray, my orthopedist shifted gears from a previous recommendation of partial knee replacement to osteotomy, which requires cutting the bone at the top of the tibia and using plates and screws to relocate it in its proper place. The one word that comes up when researching the recovery for this surgery: brutal. Standard care is crutches for two weeks and a cane for a month alongside endless physical therapy. Thanks but no thanks.
The thyroid is being an asshole, as well. Long story short: underactive thyroid, two daily meds, and two nodules that may or may not be problematic, and dissenting opinions by my crack medical team as to whether another thyroid biopsy is needed. Being the fierce player that I am, had my crack team concurred, I would have promptly had that biopsy. As much as I detest the idea of another needle being stuck IN MY NECK, I will do it if it’s necessary. But if there is dissent on the matter, I’ll defer. That said, that asshole thyroid has some wily ways of mucking up my life. Symptoms and side-effects of a wonky thyroid are far-reaching, and just when I think I have them under control (or am at least resigned to them), another one makes its grand entrance.
Which brings us to the third challenge: carpal tunnel syndrome. For a couple of years I’ve had what I thought was neuropathy: tingling, numbness, swelling, and radiating pain in both hands especially first thing in the morning. It came to a head shortly after we moved into our new house last year, and my GP chalked it up to overuse of my hands and forearms from packing and unpacking endless boxes. A round of steroids and some anti-inflammatories should have done the trick, but instead there is a fresh new hell to endure. 
Ugh.
If I employ the “coulda/woulda/shoulda” tactic for dealing with the three most-pressing physical challenges, I find myself regretting my decision to put off treatment even though I had met that $6,000 deductible last year. As I face the blank slate of a reset deductible, I wish I’d sucked it up and had the surgeries and procedures I need. Perhaps I would not be typing this very post with pins & needles fingers. Perhaps I would not be thinking about how stiff and sore my knee will be after sitting at my desk to compose a blog post. Perhaps I would not be chiding myself for having been tapped out by the end of 2014.
Cue the mental side of dealing with a physical issue. Because I did not have these problems surgically repaired, I must figure out how to change my thinking. For instance, I give myself a pep talk on the way to the gym. It goes something like this:
“Don’t think about what you used to be able to do, but focus on what you can still do.”
“You’re here.”
“Lots of people more able-bodied than you aren’t even trying.”
“Don’t look at what the other gym-rats are accomplishing; comparison is the thief of joy.”
“Even a shitty workout is better than no workout at all.”
I’m not very good at this part. I recall the words of my favorite yoga teacher: where my mind goes, so too goes my energy. I envision my faulty parts bathed in a warm glow of healing energy. But it’s work. A lot of work. I’m not a fan of listening to my body and accepting limitations; I much prefer to push through the pain. It’s a struggle to avoid falling into the “haven’t I suffered enough??” mentality, and it’s certainly not a great way to start a new year. But, instead of deciding that this old dog can’t learn a new trick, I will become a player (albeit not a starter) in this mental game. As the great Yogi Berra once said, “Ninety percent of this game is half mental.”
#nofilter
Posted: November 6, 2014 Filed under: Uncategorized | Tags: carpal tunnel syndrome, Dog from Up, funny bone, micobacterium fortuitum, nerve conduction velocity test, neurological testing for ADD, post-mastectomy infection, PTSD, PTSD from cancer, Squirrel! 10 CommentsWhat kind of moron schedules an appointment with a new specialist while recovering from yet another revision to breast reconstruction? Probably the same moron who thinks yet another revision is no big whoop and expects recovery to be swift. Will I never learn??? And the post-surgery antibiotics are wreaking their usual havoc and using black magic to cause me — a non-meat-eater and pet-pig owner — to crave ham. Ham. Of all things.
Dr E, the neurologist I saw yesterday for the mystery neuropathy I’ve been having in my hands, offices in the medical plaza adjoining the hospital to which I was admitted in early June 2010 for the nefarious post-mastectomy infection. A small PTSD episode may or may not have occurred inside that plaza at 8:30 a.m. yesterday, in which I stepped on to the wrong elevator en route to Dr E’s office and found myself not in the plaza but on the 9th floor of the hospital. I was transfixed and rooted in place, knowing I was not in the right spot but temporarily unable to grind the right gears and get out of there. I stood there, sweating profusely and shivering alarmingly near a giant window overlooking the freeway that leads from the hospital back to my home, in the Land of Sugar. The dregs of a rainy-day morning rush hour in Houston creeped along that freeway as I watched it, momentarily paralyzed with the searing memory of looking out that window on day 6 or 7 of that hellish hospitalization. My kids had just finished their second- and fifth-grade years of school; I had turned 41 just a week before that hellish hospitalization. Summer glistened ahead of us as I began a protracted and ugly battle against a rare and nasty infection following a cruel and unexpected cancer diagnosis. If someone had predicted that nearly 5 years later I would be paralyzed simply by being in that same hospital, I would have rolled my eyes and scoffed at that lame-0 idea. Suffice to say, no eye-rolling or scoffing occurred.
 I sweated and cursed the small, airless room. I wondered how much time had elapsed. I wondered if clicking that button was contributing to the neuropathy in my hands. I rebelled against the test directions to avoid looking for a pattern and guessing when to click the button. I composed a grocery list. I fashioned a crude fan from a piece of paper to stir the hot, stale air, not once taking my eyes off that blasted screen. I thought about what to serve my kids for dinner that constituted a nutritious meal yet required little or no work from me. I vowed to ace that test, but grew bored of and distracted from it post haste. Hence the no filter.
I sweated and cursed the small, airless room. I wondered how much time had elapsed. I wondered if clicking that button was contributing to the neuropathy in my hands. I rebelled against the test directions to avoid looking for a pattern and guessing when to click the button. I composed a grocery list. I fashioned a crude fan from a piece of paper to stir the hot, stale air, not once taking my eyes off that blasted screen. I thought about what to serve my kids for dinner that constituted a nutritious meal yet required little or no work from me. I vowed to ace that test, but grew bored of and distracted from it post haste. Hence the no filter.But instead, I was like this (pardon the profanity; it’s fitting and again, another example of me having no filter):
A terrible, horrible, no good, very bad day
Posted: October 29, 2014 Filed under: cancer fatigue, drugs | Tags: Alexander and the Terrible, Aromasin, aromatase inhibitors, Horrible, Judith Viorst, No Good, O magazine, Very Bad Day 10 CommentsTo quote from Alexander, the hero of Judith Viorst’s timeless children’s book, today was a “terrible, horrible, no good, very bad day.” 
Actually, truth be told, it’s been a terrible, horrible, no good very bad month. It’s been a death-by-a-million-paper-cuts month.
I didn’t wake up with gum in my hair or miss out on dessert at lunch like poor Alexander did. But it’s still been a THNGVB day.
This is dangerous territory. As a cancer “survivor” I should be grateful. I should be happy. I should be thankful to be alive and (more or less) in one piece.
To which I say, screw the “shoulds.”
Of course I’m grateful to have “survived” cancer (and of course I recognize that the “surviving” only hold true until the day in any given month in any given year that the cancer comes back. Which it does for some 40 percent of women diagnosed with early-stage, favorable breast cancer). I am happy that I’m not currently metastatic. I am thankful to be alive. None of this, however, cancels out the rest of the yucky stuff involved, and sometimes a girl’s gotta vent.
Today was the tipping point of my THNGVB month. A punctured tire this morning turned today’s to-do list into a scrap in the recycle bin. A cut on my leg from two weeks ago has become red, hot, painful, and pussed instead of healed. My attempts to slather it in Neosporin and cover it with a band-aid didn’t cut it (heh heh) so I’m now back in antibiotic hell. Cue the nausea, thrush, and terrible taste in my mouth, which join the dizziness, joint pain, neuropathy, fatigue, mental fog, muscle weakness, hot flashes, and sweating. Sheesh. I mean, sheesh.
I’ve been blaming this fresh hell on Aromasin, the latest aromatase inhibitor I’ve been taking to stave off a recurrence of my cancer and (theoretically) live a longer life. However, I’ve had the luxury of being off the dreaded Aromasin for a two-week period in advance of and following surgery. Yes, another surgery. Don’t be jealous. Perhaps it takes more than a two-week window to rid oneself of the nastiness Aromasin brings. Perhaps I’m just a whiner. Either way, I don’t feel good and I firmly believe that in some cases, the cure is worse than the disease.
Attempts to ameliorate any one of these symptoms are for naught. Taking a probiotic. Counting my blessings. Backing off of the intensity of my workouts. Viewing photos of baby donkeys and Golden Retriever puppies. Lighting a yummy-smelling candle. Drinking more water. Making an appointment with a neurologist. Doing a good deed for a friend in need. Nothing is helping. Nada. Nuttin.
In my most recent attempt to carve out a moment of not-hell, I read this quote in the current edition of Oprah’s magazine:
In our day-to-day lives, it’s easy to become overwhelmed with responsibilities and challenges. Having enough time to give to everybody who needs you and have any left for yourself is a constant struggle. But in the long run, designing space for you is the only way you can survive without burnout and resentment. There is no life without a spiritual life, and spirituality is like a muscle. It must be fueled. Fuel yourself with beauty, inspiration, music, laughter, nature, a hot soaking bath, silence. Whatever form it takes for you. Know this for sure: You have more to give when your own tank is full.
Dammit, Oprah! I’m trying. I’m trying to design space for me and to fuel myself. But what does one do when nothing is working?
I suppose I’ll have to take a page from Alexander’s book and move to Australia.